Abstract
Objective: To describe the health characteristics, condition-specific measures, chronic disease risk factors, and healthcare and medication use over time of individuals with musculoskeletal conditions awaiting orthopaedic surgical consultation.
Study importance: Musculoskeletal conditions are highly prevalent in the general population and often coexist with chronic diseases. However, little is documented about the overall health of this group. This study describes the health of these individuals, with particular emphasis on modifiable risk factors of chronic disease.
Study type: A repeated measures longitudinal cohort study of individuals referred for orthopaedic consultation across three time points (2014, 2015 and 2016).
Methods: This study was undertaken in the orthopaedic outpatient service of a public tertiary referral hospital in New South Wales, Australia. Participants were aged 18 years and older and were referred for and awaiting orthopaedic surgical consultation for a musculoskeletal condition (back, neck, hand or wrist pain, or hip or knee osteoarthritis). Measures included patient demographics, condition-specific indicators (e.g. pain, disability, quality of life [QoL]) and chronic disease risk factors (e.g., excess weight, smoking).
Results: The mean age of participants was 57.7 years, and 7.3% identified as Aboriginal and/or Torres Strait Islander. Back (43.1%) and knee (35.0%) pain were the most prevalent conditions. At baseline (N = 1052), participants reported moderate pain (mean numerical pain rating scale score of 6.4, standard deviation [SD] 2.4) and QoL (Physical Component Score of 32.7, SD 10.7; Mental Component Score of 46.6, SD 13.3). Chronic disease risk factors were highly prevalent, with 74.6% of participants having three or more. For most measures, there were only small changes over time.
Conclusion: Individuals with musculoskeletal conditions who are awaiting orthopaedic surgical consultation have a complex clinical picture and numerous chronic disease risk factors. Given the modifiable nature of many of these risk factors, identifying and addressing them before or while awaiting consultation may improve the health of these individuals.
Full text
Introduction
Musculoskeletal conditions are a common health issue that results in significant personal, economic and societal costs.1 In 2020–21 approximately seven million individuals in Australia had a musculoskeletal condition.2 The most common conditions in Australia are osteoarthritis (OA) of the knee and hip, and spinal pain (low back and neck pain).3
Musculoskeletal conditions are responsible for substantial health service use. In the financial year 2021–22, Australia’s most populated state, New South Wales (NSW), had 143 299 hospitalisations for musculoskeletal diseases.4 Up to 18 in every 100 individuals with musculoskeletal conditions are referred to orthopaedic specialists.5 Waiting periods for specialist care can be months or years for this group who are at risk of poor health6,7, so it is essential to understand their ongoing health needs.
Individuals with musculoskeletal conditions often have multiple health needs. In Australia, more than 60% of individuals with a musculoskeletal condition have at least one other chronic condition (e.g. diabetes mellitus), which impacts the trajectory and management of their musculoskeletal condition.8 National and international data indicate that musculoskeletal disorders and chronic diseases often coexist, leading to the poorer health of many people in the general population.7 Chronic disease risk factors include excess weight, poor diet, risky alcohol intake, smoking and physical inactivity.9 These factors contribute significantly to an individual’s health10, and may lead to higher hospitalisation rates and impact on surgical and non-surgical outcomes for individuals with musculoskeletal conditions.11 Indeed, up to 29% of patients undergoing total knee arthroplasty have unfavourable outcomes, including limited change to physical function.12 Observational data show that modifiable risk factors such as body mass index (BMI) and comorbidity potentially contribute to poorer outcomes.13
Currently, there is limited information about the health of people referred for specialist orthopaedic consultation at public hospitals in Australia. It is recommended that a trial of conservative management takes place before referral to public orthopaedic services, with the aim of a referral being to assess if surgical intervention will be beneficial. Many referred patients have lengthy waiting times for consultation, and no data describe the health risks and changes for patients while they wait. Given the volume of referrals for public orthopaedic services and the known links between modifiable health risks and outcomes of non-surgical and surgical interventions, a better understanding of the health profile in this patient group is needed. This information may provide evidence for opportunistic management that could occur before or when individuals are awaiting orthopaedic consultation.
The main objective of this study was to describe the health, condition-specific indicators (e.g. pain, disability, quality of life (QoL)) and chronic disease risk factors of people with musculoskeletal conditions awaiting orthopaedic surgical consultation over a three-year period. A secondary objective was to describe previous healthcare and medication use.
Methods
Study design, setting and participants
We used data from a longitudinal cohort study of individuals referred for orthopaedic surgical consultation. The study was part of a local audit to monitor referrals, waiting times and patient care before accessing orthopaedic services at one public tertiary referral hospital in NSW, Australia. We captured data at three time points between 2014 and 2016. Our study was approved by the Hunter New England Local Health District (HNELHD) Human Research Ethics Committee (Approval No. 13/12/11/5.18) and the University of Newcastle Human Ethics Committee (Approval No. H-2015-0043).
Eligibility and enrolment
Patients were eligible if they were on the orthopaedic outpatient waiting list at the only tertiary referral hospital within HNELHD, indicated that they still required an orthopaedic consultation, were aged 18 years and older, spoke English, and gave consent for ongoing contact and for their information to be used for research. All patients on the waiting list for an orthopaedic consultation for back, neck, hand, wrist, hip or knee pain were sent a study information letter inviting them to participate. We then contacted patients by phone to obtain verbal consent. Patients were ineligible if they were physically or mentally incapable of completing the survey or no longer needed an orthopaedic appointment (i.e. their condition had improved or care was received elsewhere). We invited new patients referred to the waitlist between the initial (2014) and second survey (2015) into the study. New patients added to the waitlist after the second survey were not eligible. Some patients referred to the service had urgent clinical needs and were booked immediately for an appointment. Because these patients were not added to the waitlist, they were not eligible for inclusion in the study.
Data collection and follow-up procedures
Participants had the opportunity to complete a baseline survey in 2014 or 2015. We then contacted consenting participants to complete a follow-up survey 12 months after their baseline survey (performed in 2014 or 2015). Participants enrolled in 2014 had two follow-up surveys (12-month and 24-month follow-up), while patients enrolled in 2015 had one follow-up survey (12-month follow-up only). Patients with an initial orthopaedic consultation during the follow-up period were still contacted for follow-up. Telephone interviewers conducted all interviews using computer-assisted telephone interviewing. Interviewers attempted up to 10 calls across multiple days and times before patients were deemed ‘uncontactable’.
Measures
We collected the following data:
- Patient demographics (e.g. age, gender)
- Condition-specific outcomes (e.g. pain intensity, disability)
- Patient health characteristics (e.g. QoL, comorbidities)
- Chronic disease risk factors (e.g. BMI, nutrition, physical activity, smoking status, alcohol consumption)
- Current healthcare and medication use
- Previous care received.
See Supplementary File 1 for a complete list of survey items (available from: osf.io/t5qy7).
Statistical analysis
For analysis, we combined data from different years into three time points: baseline, 12-month, and 24-month follow-up. We used SAS 9.3 software (SAS Institute Inc., Cary, North Carolina, US) for all statistical analyses. We present descriptive statistics for all outcomes at baseline and follow-up. We report mean, standard deviation (SD) or median, and interquartile range (IQR) to describe continuous variables and frequency counts and percentages for categorical variables. We calculated the means and 95% confidence intervals (CIs) at baseline and follow-up for condition-specific measures and patient health characteristics.
We categorised patients as being ‘at risk’ or ‘not at risk’ for non-communicable chronic diseases based on thresholds published in clinical guidelines for key preventable chronic disease risk factors.14-16 See Supplementary File 2 for ‘at risk’ classifications (available from: osf.io/t5qy7).
Results
Sample
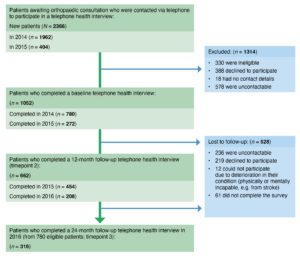
In 2014 and 2015, 2366 people were awaiting orthopaedic consultation. At baseline, 330 individuals were ineligible to participate in the study based on the exclusion criteria, 388 declined to participate, 578 were uncontactable, and 18 were not contacted as their contact details were not collected. We collected baseline data from 1052 participants (780 in 2014, 272 in 2015). Of those participants who completed a baseline survey, 662 (62.9%) completed a 12-month follow-up (i.e. provided data for two time points). Of the 780 enrolled participants in 2014, 316 (40.5%) completed a 24-month follow-up (i.e. provided data for three time points). Figure 1 shows the flow of participants through the study.
Figure 1. Flow of participants through the study (click on figure to enlarge)
Baseline characteristics
The mean age of patients who completed the baseline survey was 57.7 years (SD 14.5). Most participants (59.2%) were female, and 7.3% identified as Aboriginal and/or Torres Strait Islander (Table 1). The most commonly reported locations of primary musculoskeletal complaints were the back (43.1%) and/or knee (35.0%). More than 80% of individuals reported a coexisting medical condition that required medication.
Table 1. Baseline characteristics
| Variable | (N = 1052) |
| Age (years), mean (SD) | 57.7 (14.5) |
| Gendera, n (%) | |
| Female | 622 (59.2) |
| Male | 428 (40.8) |
| Employment status, n (%) | |
| Employed | 248 (23.6) |
| Unemployed | 186 (17.7) |
| Retired | 378 (35.9) |
| Can’t work (health reasons) | 240 (22.8) |
| Country of origin (Australia), n (%) | 928 (88.2) |
| English not spoken at home, n (%) | 26 (3.3) |
| Other coexisting medical conditions needing medication (three most common), n (%) | 852 (81.0) |
| Hypertension | 416 (46.3) |
| Arthritisb | 356 (39.6) |
| Depression, anxiety, stress | 332 (36.9) |
| Time (days) from initial referralc, median (IQR) | 560 (345–998) |
| Locally defined triage classificationd, n (%) | |
| Urgent | 122 (14.0) |
| Semi-urgent | 702 (80.4) |
| Non-urgent | 49 (5.6) |
| Location of primary complaint, n (%) | |
| Back pain | 465 (43.5) |
| Neck pain | 34 (3.2) |
| Knee osteoarthritis | 374 (35.0) |
| Hip osteoarthritis | 88 (8.2) |
| Hand pain | 109 (10.2) |
| Multisite paine | 825 (78.5) |
| Pain intensity (NPRS), mean (SD) | 6.4 (2.4) |
| Pain duration (years), median (IQR) | 5.0 (2.5–15.0) |
IQR = interquartile range; NPRS = numeric pain rating scale; SD = standard deviation.
a Two participants did not respond to gender question.
b Arthritis that is not the subject of the individual’s referral. For example, if participants were referred for hip osteoarthritis but were also told that they had knee osteoarthritis requiring medication, they were classified as having arthritis as a coexisting medical condition.
c Calculated from date of referral to date of contact by study interviewers.
d Triage classifications may have changed subject to changes in a patient’s presentation.
e Multisite pain refers to participants who were referred for a primary complaint (e.g. back pain) but also reported pain in other sites.
Health characteristics and condition-specific outcomes
For patients with back pain and osteoarthritis (OA), the baseline mean scores for the Roland–Morris Disability Questionnaire (RMDQ) and the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) were 15.2 out of 24 (95% CI 14.2, 16.2) and 46.1 out of 96 (95% CI 42.6, 49.5), respectively. RMDQ scores of 9–16 indicate moderate disability while increasing WOMAC scores indicate worse pain, stiffness and functional limitations. At baseline, the mean BMI was 30.3 kg/m2 (SD 6.9), with 72.5% of participants classified as overweight or obese. We observed small improvements in most condition-specific measures and patient health characteristics across the three time points (e.g. the mean RMDQ at baseline was 15.2, compared to 13.2 at 24 months). Further details are described in Table 2.
Table 2. Patient health characteristics and condition-specific measures
| Measure (scale) | At baselinea | At 12 months | At 24 months |
| Condition-specific measures, mean (95% CI) | |||
| RMDQ (0–24)b | 15.2 (14.2, 16.2) (n = 143) |
14.1 (13.4, 14.8) (n = 332) |
13.2 (12.0, 14.3) (n = 141) |
| WOMAC (0–96)b | 46.1 (42.6, 49.5) (n = 127) |
43.8 (41.1, 46.5) (n = 246) |
38.3 (33.7, 43.0) (n = 109) |
| Örebro MPQ (0–100)b | Not collected | 58.7 (55.4, 61.9) (n = 79) |
45.8 (41.3, 50.3) (n = 62) |
| Pain intensity (NPRS) (0–10)b, mean (95% CI) | 6.4 (6.2, 6.5) (n = 1048) |
6.0 (5.8, 6.2) (n = 659) |
4.9 (4.6, 5.3) (n = 312) |
| Quality of life (SF12v2), mean (95% CI) | |||
| PCS (0–100)c | 32.7 (32.1, 33.4) (n = 989) |
33.2 (32.2, 34.1) (n = 623) |
35.1 (33.8, 36.3) (n = 314) |
| MCS (0–100)c | 46.6 (45.8, 47.5) (n = 989) |
48.8 (47.8, 49.7) (n = 623) |
48.8 (47.4, 50.2) (n = 314) |
| Beliefs, mean (95% CI) | |||
| FABQPA (0–24)b | 16.7 (16.0, 17.5) (n = 270) |
15.9 (15.3, 16.4) (n = 657) |
13.7 (12.8, 14.5) (n = 313) |
| Mental health, mean (95% CI) | |||
| Depression Anxiety Stress Scale (DASS21)b | 15.6 (14.1, 17.1) (n = 269) |
15.2 (14.3, 16.2) (n = 659) |
14.4 (13.1, 15.7) (n = 311) |
| Depression (0–21)b | 5.2 (4.6, 5.8) (n = 270) |
5.1 (4.7, 5.5) (n = 660) |
4.7 (4.1, 5.2) (n = 311) |
| Anxiety (0–21)b | 4.1 (3.7, 4.6) (n = 269) |
4.1 (3.8, 4.4) (n = 660) |
4.0 (3.5, 4.4) (n = 311) |
| Stress (0–21)b | 6.2 (5.6, 6.8) (n = 270) |
6.0 (5.7, 6.4) (n = 659) |
5.8 (5.3, 6.3) (n = 311) |
| Weight (kg), mean (95% CI) | 85.6 (84.4, 86.9) (n = 1032) |
87.8 (86.1, 89.4) (n = 655) |
85.0 (82.7, 87.2) (n = 315) |
| BMI (kg/m2), mean (95% CI) | 30.3 (29.9, 30.7) (n = 995) |
31.0 (30.5, 31.6) (n = 633) |
29.8 (28.9, 30.7) (n = 315) |
| Moderate-to-vigorous physical activity (minutes/week), mean (95% CI) | 73.5 (63.8, 83.2) (n = 1031) |
86.1 (73.1, 99.2) (n = 643) |
86.8 (69.3, 104.3) (n = 300) |
| Alcohol consumption (AUDIT score) (0–12)b, mean (95% CI) | 2.7 (2.5, 2.9) (n = 1048) |
2.5 (2.3, 2.8) (n = 660) |
2.6 (2.3, 2.8) (n = 312) |
| Sleep quality (1–4)d, mean (95% CI) | 2.7 (2.6, 2.8) (n = 272) |
2.6 (2.6, 2.7) (n = 662) |
2.6 (2.5, 2.7) (n = 316) |
| Smoked in the last 4 weeks (yes), n (%) | 241 (22.9) (N = 1052) |
135 (20.4) (N = 661) |
57 (18.2) (N = 313) |
| Fruit serves/day, n (%) | (N = 1044) | (N = 662) | (N = 316) |
| 0–1 | 502 (48.0) | 334 (50.5) | 142 (44.9) |
| 2 or more | 545 (52.1) | 328 (49.6) | 174 (55.1) |
| Vegetable serves/day, n (%) | (N = 1044) | (N = 662) | (N = 316) |
| 0–2 | 449 (43.0) | 284 (42.9) | 125 (39.6) |
| 3–4 | 416 (39.8) | 263 (39.7) | 124 (39.2) |
| 5 or more | 179 (17.1) | 115 (17.4) | 67 (21.2) |
AUDIT = Alcohol Use Disorders Identification Test; BMI = body mass index; FABQPA = Fear-Avoidance Beliefs Questionnaire, physical activity subscale; MCS = Mental Component Score; NPRS = numeric pain rating scale; Örebro MPQ = Örebro Musculoskeletal Pain Questionnaire; PCS = Physical Component Score; RMDQ = Roland–Morris Disability Questionnaire, which is a low back pain measure; SF12v2 = Short-Form 12-Item Survey (version 2); WOMAC = Western Ontario and McMaster Universities Osteoarthritis Index.
a The total responses for the baseline survey may not equal the total available for all variables, as some variables were only added to the survey in 2015.
b Higher scores indicate worse symptoms.
c Lower scores indicate worse symptoms.
d The sleep quality rating ranges from 1 (very good) to 4 (very bad).
Prevalence of chronic disease risk factors
Table 3 shows the prevalence of ‘at risk’ chronic disease risk factors. The median number of chronic disease risk factors (3, IQR 2–4) remained stable across the three time points. The percentage of patients with three or more risk factors decreased from 74.6% at baseline to 69.9% at the third time point. Less than half of all participants recalled being told by a healthcare provider of the benefits of addressing individual chronic disease risk factors. Approximately one in four (25.3%) had not attempted to improve their relevant risk factors (Table 3).
Table 3. Prevalence of chronic disease risk factors
| Variable | At baseline | At 12 months | At 24 months |
| Number of risk factors, median (IQR) | 3 (2–4) (N = 1052) |
3 (2–4) (N = 662) |
3 (2–4) (N = 316) |
| BMI at risk, n (%) | 720 (72.5) (N = 993) |
476 (75.4) (N = 631) |
222 (70.5) (N = 315) |
| Lost or gained weight while on waitlist, n (%) | (N = 779) | (NC) | (NC) |
| Lost weight | 282 (36.2) | NC | NC |
| Gained weight | 206 (26.4) | NC | NC |
| Neither | 274 (35.2) | NC | NC |
| Told of benefits of losing weight, n (%) | 388 (49.7) (N = 780) |
NC | NC |
| Referred to a diet or weight loss group, n (%) | 93 (12.2) (N = 764) |
NC | NC |
| Interested in losing weight, n (%) | 494 (63.3) (N = 780) |
NC | NC |
| Have physical inactivity (<150 min MVPA/week), n (%) | 868 (87.4) (N = 993) |
518 (78.5) (N = 660) |
235 (75.3) (N = 312) |
| Told of benefits of increasing activity, n (%) | 344 (44.1) (N = 780) |
NC | NC |
| Referred to physical activity group, n (%) | 116 (14.9) (N = 780) |
NC | NC |
| Interested in increasing activity, n (%) | 491 (62.9) (N = 780) |
NC | NC |
| Nutrition, n (%) | |||
| <2 serves of fruit a day | 502 (47.9) (N = 1047) |
322 (48.7) (N = 661) |
143 (45.8) (N= 312) |
| <5 serves of vegetables a day | 865 (82.9) (N= 1044) |
544 (82.3) (N= 661) |
261 (83.7) (N = 312) |
| Told of benefits of improving diet, n (%) | 327 (41.9) (N = 780) |
NC | NC |
| Interested in improving diet, n (%) | 452 (57.9) (N = 780) |
NC | NC |
| Overconsumes alcohol (AUDIT score ≥6), n (%) | 194 (18.5) (N = 1048) |
108 (16.4) (N = 660) |
42 (13.5) (N = 312) |
| Told of benefits of reducing alcohol, n (%) | 64 (24.2) (N = 265) |
NC | NC |
| Interested in reducing alcohol, n (%)a | 73 (27.9) (N= 262) |
NC | NC |
| Is a smoker (smoked in the last 4 weeks), n (%) | 241 (22.9) (N= 1052) |
135 (20.4) (N = 661) |
57 (18.2) (N = 313) |
| Told of benefits of quitting smoking, n (%) | 93 (54.7) (N= 170) |
NC | NC |
| Interested in quitting smoking, n (%)a | 121 (71.6) (N = 169) |
NC | NC |
| Tried to reduce risks, n (%)b | 583 (74.7) (N = 780) |
NC | NC |
| Tried to reduce alcohol intake, n (%) | 108 (41.1) (N = 263) |
NC | NC |
| Tried to reduce smoking, n (%) | 66 (38.8) (N = 170) |
NC | NC |
| Has three or more ‘at risk’ health risk factors, n (%) | 785 (74.6) (N = 1052) |
487 (73.6) (N = 662) |
221 (69.9) (N = 316) |
AUDIT = Alcohol Use Disorders Identification Test; BMI = body mass index; IQR = interquartile range; MVPA = moderate-to-vigorous physical activity; NC = not collected.
a Includes participants who were ‘interested’ and ‘very interested’.
b Includes through changing weight, physical activity and diet.
Provision of care before referral and while awaiting orthopaedic surgical consultation
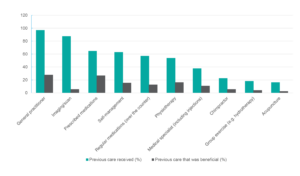
Imaging and medications prescribed by general practitioners (GPs) were the types of care most frequently accessed by patients on the waitlist. Figure 2 shows the 10 most commonly reported types of previous care accessed by patients and the percentage of patients who found that care beneficial. While many patients had accessed a variety of healthcare options, patients mostly found these to be not beneficial. For example, only 28.0% and 16.4% of the sample found GP and physiotherapy care beneficial, respectively. For further details, see Supplementary File 3, available from: osf.io/t5qy7.
Current medication and healthcare use were variable (see Supplementary File 4, available from: osf.io/t5qy7). The most common medication currently being used by patients was paracetamol (used by 37.5% of all participants). Opioid use appeared constant across the three time points, with approximately 20% of participants indicating that they were currently using an opioid. GPs were the health professionals most often seen in the previous 6 weeks (ranging from 23.7% to 32.4% across the three time points) followed by physiotherapists (ranging from 3.8% to 8.1% across the three time points).
Figure 2. Type of previous care received and perceived benefit of care (click on figure to enlarge)
Discussion
We describe the characteristics and health course of patients who were referred for and awaiting orthopaedic surgical consultation for musculoskeletal conditions. This patient group had been feeling pain for a considerable length of time at baseline (median duration of 5 years). Disability, QoL, and other condition-specific measures indicated that this patient group had moderately impacted health, which only improved slightly across follow-up. Chronic disease risk factors were highly prevalent and remained constant over time. Approximately three-quarters of patients had at least three risk factors, with more than 70% of patients at risk according to BMI and inactivity, 80% at risk based on nutrition, and there was almost double the national prevalence of smoking. While most participants reported an interest in addressing chronic disease risk factors, few reported receiving advice or care. The majority of participants reported that previous care for their musculoskeletal condition had not been beneficial.
The health of individuals awaiting orthopaedic surgical consultation for musculoskeletal conditions within the Australian public health system is worse than the general population. Compared with the general Australian population and 2016 HNELHD data, individuals referred to orthopaedic specialists were more likely to have a high BMI (72.5% compared with 67.0% and 60.3%)4,17, smoke daily (22.9% compared with 11.6% and 11.7%)4,18 and have low physical activity levels (82.5% compared with 55.0% and 48.2%)4,19. However, they were less likely than the general Australian population to consume risky amounts of alcohol (18.5% compared with 25.8%).20 Due to the relationship between musculoskeletal conditions and chronic diseases8, it is possible that the high rate of chronic disease risk factors in this patient group may also affect their clinical presentation. No other studies have described the prevalence of chronic disease risk factors or the previous care this patient group received, particularly over multiple time points. Our study found that condition-specific QoL and WOMAC scores improved slightly over time, unlike Ackerman et al.21, who found that scores deteriorated in patients awaiting a total hip or knee replacement. However, Ackerman and colleagues21 included patients awaiting total knee or hip arthroplasty, with 68% of their sample having an operation within 12 months. In comparison, our sample consisted of various musculoskeletal conditions that had not yet had an initial consultation. It was likely that many of these patients did not go on to have surgery following their consultation.
While previous studies have a cross-sectional design or short follow-up period21,22, our study provides a clinical picture of the orthopaedic outpatient waitlist across a 3-year period. We attempted to sample all patients from the waiting list, which accepts referrals for patients living in metropolitan, regional and rural areas across HNELHD. The health district covers an area of 131 785 km2 in eastern and northern NSW, Australia.
We do not know if the health of those who were uncontactable (n = 578) or of those excluded as they did not speak English differs from our study sample. Our study did not include all musculoskeletal presentations (e.g. shoulder, elbow, ankle, foot), and it is unknown whether the findings of this study are generalisable to those presentations. This study only considered patients referred for orthopaedic surgical consultation at a public hospital; patients referred to other specialty groups and private services were not included. Due to the survey’s self-reported nature, there may be an element of recall bias; however, most questions used a recent time frame (e.g. past 4–6 weeks) to overcome this.
Patients waiting for orthopaedic surgical consultation for musculoskeletal conditions have a variety of health issues alongside their presenting condition. Patients in our study waited for a median time of 560 days from referral to the time they were contacted as part of this study. While awaiting orthopaedic surgical consultation, these patients sit in the grey area between primary and secondary care, often with no or minimal care, especially for modifiable chronic disease risk factors. While programs like the Osteoarthritis Chronic Care Program23 may provide some support for these patients, such programs are not available in all areas. They may not be accessible to patients until much later in their care pathway (i.e. upon recommendation for elective surgery). Currently, there are limited service options for the large number of people referred and waiting for initial consideration of surgery.
People with musculoskeletal conditions, including those in the general community, need support to address modifiable health risk factors. In Australia, extended waiting periods for some patients provide an untapped opportunity to address health and chronic disease risk factors. With growing evidence highlighting the role of health risk factors in chronic disease development and poor outcomes in both the general population and patients with OA and spinal pain24,25, intervention during waiting periods may have multiple effects. It may reduce the risk of chronic diseases or the number of hospitalisations for an individual’s chronic diseases. It may also improve patient and health system outcomes related to the surgical process. For example, providing preventive care services earlier in the course of care may reduce the risk of related surgical complications or reduce the need for surgery.7,11 Given the high prevalence of chronic disease risk factors and the extended waiting periods, active support during this time is an opportunity to reach a population group at high risk of ongoing poor health.
Future research should explore how the health system can be improved to support patients during extended waiting times. The current separation of care between primary and secondary care also needs attention to identify who within the health system is best placed to provide care for chronic disease risk factors and facilitate better care integration. Integration will help avoid patients being ‘lost’ between the systems. With the increasing demand on GPs5, we may see more unmet primary health concerns within secondary care. Research should examine how population-based services (e.g. Quitline, Get Healthy Service) and allied health (e.g. physiotherapy, dietetics) can be used to care for chronic disease risk factors for individuals with musculoskeletal conditions. Research should also seek to understand why individuals awaiting orthopaedic surgical consultation do not regularly access allied health professionals before or during waiting periods.
Conclusion
Patients referred to orthopaedic specialists have multiple modifiable risks for chronic diseases. These risks may contribute to the progression of their musculoskeletal condition and explain their poorer overall health compared with the general population. Patients are not actively supported to manage these risks during their long waiting times, which represents an untapped opportunity to improve the health of these people.
† Population Health Working Group (consortium authorship) includes:
Dr Amanda Williams – School of Medicine and Public Health, University of Newcastle
Professor John Wiggers – School of Medicine and Public Health, University of Newcastle; Population Health, Hunter New England Local Health District; Hunter Medical Research Institute
Ms Karen Gillham – Population Health, Hunter New England Local Health District; Hunter Medical Research Institute
Dr Elizabeth Campbell – School of Medicine and Public Health, University of Newcastle; Population Health, Hunter New England Local Health District; Hunter Medical Research Institute.
Mr Christophe Lecathelinais – Population Health, Hunter New England Local Health District; Hunter Medical Research Institute.
Acknowledgements
CW and SK receive salary funding from the Australian National Health and Medical Research Council.
Peer review and provenance
Externally peer reviewed, not commissioned.
Copyright:
© 2023 Davidson et al. This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International Licence, which allows others to redistribute, adapt and share this work non-commercially provided they attribute the work and any adapted version of it is distributed under the same Creative Commons licence terms.
References
- 1. Hartvigsen J, Hancock MJ, Kongsted A, Louw Q, Ferreira ML, Genevay S, et al. What low back pain is and why we need to pay attention. Lancet. 2018;391(10137):2356–67. CrossRef | PubMed
- 2. Australian Institute of Health and Welfare. Chronic musculoskeletal conditions. Canberra: AIHW; 2023 [cited 2023 Nov 15]. Available from: www.aihw.gov.au/reports/chronic-musculoskeletal-conditions/musculoskeletal-conditions/contents/summary.
- 3. Vos T, Abajobir AA, Abate KH, Abbafati C, Abbas KM, Abd-Allah F, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. 2017;390(10100):1211–59. CrossRef | PubMed
- 4. Centre for Epidemiology and Evidence. HealthStats NSW Sydney: NSW Ministry of Health [cited 2022 Nov 1]. Available from: www.healthstats.nsw.gov.au/#/r/102814
- 5. Brand CA, Harrison C, Tropea J, Hinman RS, Britt H, Bennell K. Management of osteoarthritis in general practice in Australia. Arthritis Care Res (Hoboken). 2014;66(4):551–8. CrossRef | PubMed
- 6. Frank AO, De Souza LH, McAuley JH, Sharma V, Main CJ. A cross-sectional survey of the clinical and psychological features of low back pain and consequent work handicap: use of the Quebec Task Force classification. Int J Clin Pract. 2000;54(10):639–44. CrossRef | PubMed
- 7. Williams A, Wiggers J, O'Brien K, Lee H, Wolfenden L, Yoong SL, et al. Musculoskeletal conditions may increase the risk of chronic disease: a systematic review and meta-analysis of cohort studies. BMC Med. 2018;16. CrossRef | PubMed
- 8. Australian Institute of Health and Welfare. Musculoskeletal conditions and comorbidity in Australia. Canberra: AIHW; 2019 [cited 2023 Nov 15]. Available from: www.aihw.gov.au/reports/chronic-musculoskeletal-conditions/musculoskeletal-conditions-comorbidity-australia/summary
- 9. Dean E, Söderlund A. What is the role of lifestyle behaviour change associated with non-communicable disease risk in managing musculoskeletal health conditions with special reference to chronic pain? BMC Musculoskelet Disord. 2015;16:87. CrossRef | PubMed
- 10. Australian Institute of Health and Welfare. Australia's health 2016 fact sheet. How lifestyle choices affect our health. Canberra: AIHW; 2016 [cited 2023 Nov 15]. Available from: www.aihw.gov.au/getmedia/0ea3cb23-34c3-4e3b-8a20-8c1c0cde6586/ah16-factsheet-lifestylechoices.pdf.aspx
- 11. Levett DZH, Edwards M, Grocott M, Mythen M. Preparing the patient for surgery to improve outcomes. Best Pract Res Clin Anaesthesiol. 2016;30(2):145–57. CrossRef | PubMed
- 12. Maxwell JL, Felson DT, Niu J, Wise B, Nevitt MC, Singh JA, et al. Does clinically important change in function after knee replacement guarantee good absolute function? The multicenter osteoarthritis study. J Rheumatol. 2014;41(1):60–4. CrossRef | PubMed
- 13. Singh JA, O'Byrne M, Harmsen S, Lewallen D. Predictors of moderate-severe functional limitation after primary Total Knee Arthroplasty (TKA): 4701 TKAs at 2-years and 2935 TKAs at 5-years. Osteoarthritis Cartilage. 2010;18(4):515–21. CrossRef | PubMed
- 14. National Health and Medical Research Council. Clinical practice guidelines for the management of overweight and obesity in adults, adolescents and children in Australia. Melbourne: NHMRC; 2013 [cited 2023 Nov 15]. Available from: www.nhmrc.gov.au/about-us/publications/clinical-practice-guidelines-management-overweight-and-obesity
- 15. National Health and Medical Research Council. Australian dietary guidelines. Canberra: NHMRC; 2013 [cited 2023 Nov 15]. Available from: www.nhmrc.gov.au/adg
- 16. Brown W, Bauman A, Bull F, Burton N. Development of Evidence-based physical activity recommendations for adults (18-64 years). Canberra: Australian Government Department of Health; 2012 [cited 2023 Nov 15]. Available from: www.health.gov.au/resources/publications/development-of-evidence-based-physical-activity-for-adults-18-to-64-years?language=en
- 17. Australian Institute of Health and Welfare. Overweight & obesity. Canberra: AIHW; 2023 [cited 2023 Nov 15] Available from: www.aihw.gov.au/reports-data/behaviours-risk-factors/overweight-obesity/overview
- 18. Australian Institute of Health and Welfare. Tobacco smoking. Canberra: AIHW; 2023 [cited 2023 Nov 15]. Available from: www.aihw.gov.au/reports/alcohol/alcohol-tobacco-other-drugs-australia/contents/drug-types/tobacco
- 19. Australian Institute of Health and Welfare. Insufficient physical activity. Canberra: AIHW; 2020 [cited 2023 Nov 15]. Available from: www.aihw.gov.au/reports/risk-factors/insufficient-physical-activity/contents/about
- 20. Australian Bureau of Statistics. Alcohol consumption. Canberra: ABS; 2022 [cited 2023 Nov 15]. Available from: www.abs.gov.au/statistics/health/health-conditions-and-risks/alcohol-consumption/latest-release
- 21. Ackerman IN, Bennell KL, Osborne RH. Decline in health-related quality of life reported by more than half of those waiting for joint replacement surgery: a prospective cohort study. BMC Musculoskelet Disord. 2011;12(1):108. CrossRef | PubMed
- 22. Haskins R, Henderson JM, Bogduk N. Health professional consultation and use of conservative management strategies in patients with knee or hip osteoarthritis awaiting orthopaedic consultation. Aust J Prim Health. 2014;20(3):305–10. CrossRef | PubMed
- 23. NSW Agency for Clinical Innovation. Musculoskeletal network. Osteoarthritis chronic care program model of care. Sydney: ACI; 2012 [cited 2023 Nov 15]. Available from: aci.health.nsw.gov.au/__data/assets/pdf_file/0003/165306/Osteoarthritis-Chronic-Care-Program-Mode-of-Care-High-Resolution.pdf
- 24. Shiri R, Falah-Hassani K, Heliövaara M, Solovieva S, Amiri S, Lallukka T, et al. Risk factors for low back pain: a population-based longitudinal study. Arthritis Care Res (Hoboken). 2019;71(2):290–99. CrossRef | PubMed
- 25. Björck-van Dijken C, Fjellman-Wiklund A, Hildingsson C. Low back pain, lifestyle factors and physical activity: a population based-study. J Rehabil Med. 2008;40(10):864–9. CrossRef | PubMed