Abstract
Objectives: Skin cancer is highly preventable through primary prevention activities such as avoiding ultraviolet radiation exposure during peak times and regular use of sun protection. General practitioners (GPs) and primary care nurses have key responsibilities in promoting sustained primary prevention behaviour. We aimed to review the evidence on skin cancer primary prevention activities in primary care settings, including evidence on feasibility, effectiveness, barriers and enablers.
Study type: Rapid review and narrative synthesis.
Methods: We searched published literature from January 2011 to October 2022 in Embase, Medline, PsychInfo, Scopus, Cochrane Central and CINAHL. The search was limited to skin cancer primary prevention activities within primary care settings, for studies or programs conducted in Australia or countries with comparable health systems. Analysis of barriers and enablers was informed by an implementation science framework.
Results: A total of 31 peer-reviewed journal articles were included in the review. We identified four main primary prevention activities: education and training programs for GPs; behavioural counselling on prevention; the use of novel risk assessment tools and provision of risk-tailored prevention strategies; and new technologies to support early detection that have accompanying primary prevention advice. Enablers to delivering skin cancer primary prevention in primary care included pairing preventive activities with early detection activities, and access to patient resources and programs that fit with existing workflows and systems. Barriers included unclear requirements for skin cancer prevention counselling, competing demands within the consultation and limited access to primary care services, especially in regional and remote areas.
Conclusions: These findings highlight potential opportunities for improving skin cancer prevention activities in primary care. Ensuring ease of program delivery, integration with early detection and availability of resources such as risk assessment tools are enablers to encourage and increase uptake of primary prevention behaviours in primary care, for both practitioners and patients.
Full text
Introduction
Skin cancer, including melanoma and keratinocyte cancers (basal cell carcinomas and squamous cell carcinomas), is the most prevalent cancer in Australia.1 In addition to the impact of skin cancer diagnoses on the community, the healthcare costs are estimated to be more than A$1.68 billion annually.2
Primary prevention is the most cost-effective skin cancer control measure.3 Efforts to prevent skin cancer in Australia have included public health awareness campaigns such as the Cancer Council’s SunSmart initiatives including the Slip! Slop! Slap! campaign and a ban on commercial sunbeds, which have been linked to declining melanoma incidence rates among younger Australians since 1980.4 But Australia has a pervasive culture of outdoor activities and tanning, which results in high levels of incidental ultraviolet (UV) radiation exposure and sunburn.5 The use of well-accepted preventive measures, such as regular sunscreen use and wearing a broad brim hat, has not consistently improved since 2004.5,6
Given that primary care is often the first port of call for skin cancer concerns in the community, general practitioners (GPs) and primary care nurses have important responsibilities in skin cancer primary prevention.7 But our understanding of how primary prevention activities are currently delivered in primary care settings is limited. For example, over the past decade, skin cancer risk assessment models and tools for use in clinical practice have rapidly developed alongside improvements in knowledge about skin cancer risk factors.8 Clinical practice guidelines such as the Guidelines for preventive activities in general practice9 focus on assessing patient skin cancer risk and targeting high-risk groups for prevention and early detection activities, but evidence on implementing these recommendations in primary care is limited.
We aimed to conduct a review on skin cancer primary prevention activities that have been administered in primary care settings in Australia and other countries with comparable healthcare systems (e.g., New Zealand, UK). We considered a broad spectrum of interventions and activities, including behavioural counselling, risk assessment tools, and technologies for early detection, which can involve elements of both primary and secondary prevention. We also aimed to establish the barriers and enablers to GPs and practice nurses delivering skin cancer prevention activities.
Methods
The protocol of this review was prospectively registered in PROSPERO (CRD42022355027) and follows the reporting guidelines detailed in the PRISMA statement. This review was initially prepared as a rapid review brokered by the Sax Institute for the Cancer Institute NSW, the New South Wales (NSW) Government’s cancer control agency.10
Eligibility criteria
Studies were included if they met the following criteria:
- Included primary prevention strategies/interventions/techniques/programs
- Were based in primary care settings, involving primary care physicians and/or primary care nurses. Given that models of primary care funding and practice vary across different jurisdictions, we also included studies that were based in general practice–specific settings, involving GPs and/or practice nurses
- Included skin cancer (melanoma and/or non-melanoma skin cancer)
- Were conducted in (or included studies conducted in) Australia, UK, New Zealand, Canada, Ireland, Western Europe, Scandinavia
- Were conducted from 2011 onwards.
Studies were excluded if they:
- Were not available in English
- Had a sole focus on countries outside inclusion scope (e.g., US, African countries.)
- Were dated prior to 2011
- Did not include all three key topics: primary prevention, primary care settings, and skin cancer.
- Were systematic or scoping reviews.
Information sources
Searches were conducted on Embase, Medline, PsychInfo, Scopus, Cochrane Central and CINAHL from January 2011 to October 2022 to reflect contemporary healthcare practices and capture the developments in knowledge about skin cancer risk factors and risk assessment tools over the past decade.
Search strategy
The search strategy was developed according to the Sample, Phenomenon of Interest, Design, Evaluation, Research Type (SPIDER) tool for qualitative and mixed-methods evidence synthesis11 (see Supplementary materials for search terms, available from: doi.org/10.6084/m9.figshare.25053656.v1).
Selection process
All search results were imported into Covidence (Melbourne, Australia: Veritas Health Innovation; 2022). Duplicate search results were removed automatically by Covidence and manually by screeners. All abstracts and titles were screened by NS and AS or KD. The full text screening was completed by NS and AS. Conflicts were resolved through discussion between NS, AS, KD and AC to reach consensus.
Data items and collection process
Data from the final texts were extracted and catalogued by NS and reviewed by AS according to the relevant data items (author, year of publication, study setting, study design, description of primary prevention activities, main outcomes, effectiveness and feasibility, and barriers and/or enabler of the intervention; see Supplementary Table 1, available from: doi.org/10.6084/m9.figshare.25053656.v1).
Study quality and strength of evidence
The quality of included empirical studies was assessed using the Mixed Methods Appraisal Tool (MMAT) Version 2011. The MMAT is designed for use in systematic literature reviews that include qualitative, quantitative and mixed methods studies12, and appraises the methodological quality of studies according to criteria such as the relevance of data sources and analytical approaches (qualitative studies), the appropriateness of measurements and acceptability of response rates (quantitative studies), and the relevance of research designs and integration of data (mixed methods studies). MMAT scores range from one star (one quality criterion met) to five stars (all criteria met). As the MMAT does not apply to appraising literature reviews, we used the Critical Appraisal Skills Programme (CASP) checklist for the systematic and scoping reviews (available from: casp-uk.net/casp-tools-checklists).
Synthesis methods
All relevant information was synthesised and summarised into the data collection table (Supplementary Table 1, available from: doi.org/10.6084/m9.figshare.25053656.v1). Barriers and enablers identified in the included articles were coded according to the Consolidated Framework for Implementation Research (CFIR) to determine their frequency and provide a framework for reporting (see Supplementary Table 2, available from: doi.org/10.6084/m9.figshare.25053656.v1). We chose the CFIR to guide this synthesis as there was a wide diversity of study types and it is a pragmatic framework for identifying potential influences on the implementation of novel interventions in health systems.13
Certainty assessment
The literature search strategy was designed to include only peer-reviewed articles to ensure confidence in the evidence of reported outcomes.
Results
Study selection
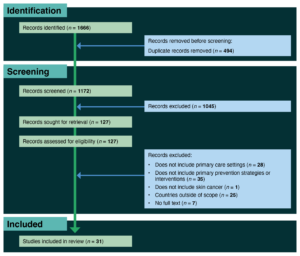
A total of 31 peer-reviewed journal articles met the eligibility criteria and were included in the review (Figure 1). Nine studies were conducted in Australia, six in the UK, and the remaining studies predominately in Europe.
Figure 1. PRISMA flow diagram (click figure to enlarge)
Study characteristics
A range of study designs and outcomes were identified, which encompassed various activities, programs and strategies relevant to primary prevention of skin cancer in primary care. Detailed study characteristics for each research article are catalogued in Supplementary Table 1, including quality criteria scores for MMAT and/or CASP according to relevant study designs (available from: doi.org/10.6084/m9.figshare.25053656.v1). Most studies fulfilled all the quality criteria specified by the MMAT according to each study design, and the articles appraised using CASP met most qualifying criteria, indicating low risk of bias in the appraised studies.
Study findings
The included studies predominately related to: 1) education and training programs for GPs; 2) behavioural counselling on prevention; 3) the use of novel risk assessment tools and provision of risk-tailored prevention strategies; and 4) new technologies to support early detection that have accompanying primary prevention advice. The results of the evidence synthesis according to these categories are described below.
1. Education and training programs for GPs
Nine research articles were related to GP knowledge, education and training on skin cancer primary prevention.7,14-21 A notable example was the Dermoscopy for Victorian General Practice Program involving 130 GP participants,7 which involved access to online training and educational models and a 1-day face-to-face training workshop (8 hours), where participants received a fully funded dermatoscope. GPs who completed the program reported they increased provision of preventive information to high-risk patients at the time of a skin examination (93%). They also felt the program had improved their quality of patient care regarding early detection of skin cancer (98.7%) and their assessment and decision making in referring patients to dermatologists (91.1%).
2. Behavioural counselling on prevention
Five articles focused on GP-delivered behavioural counselling for skin cancer primary prevention. These studies included a randomised controlled trial22, a scoping review23, two cross-sectional analyses24,25 and a qualitative interview study.26 The article by Hedevik and colleagues22 reported on a Swedish study conducted in general practice involving 309 participants, which showed those who received personalised preventive counselling and a whole body skin check from their GP significantly increased their sun protection behaviours compared with patients who only received a mailed letter containing sun protection recommendations. Although this significant difference persisted to the 10-year follow-up, engagement in sun protection behaviours decreased over time, which the authors suggest highlights the importance of repeating this type of intervention to ensure sustainability. Together these articles indicate that clinicians play an important role in counselling patients about sun protective behaviours, and tailoring messages to the age and demographics of target groups (e.g., high-risk groups) may have the greatest impact on behaviours. The qualitative interview study26 based in Australian Aboriginal primary care showed that health promotion activities including skin cancer prevention, delivered by a primary care–based cancer care team, were a culturally safe and accessible service for Aboriginal Australian clients.
3. The use of novel risk assessment tools and provision of risk-tailored prevention strategies
Twelve publications examined melanoma risk assessment in the context of primary care.8,27-37 Taken together, the intervention studies demonstrated that risk assessment using a melanoma risk prediction tool and providing corresponding prevention advice tailored to individual risk were associated with improved sun protection behaviours, and that these interventions were feasible and acceptable to participants in primary care settings.31,35,36 Undergoing melanoma risk assessment in a GP clinic, for example by using an iPad in the clinic waiting room, was found to be feasible and acceptable in Australia27,28 and the UK.29,33 A qualitative interview study demonstrated that Australian GPs were largely receptive to the use of melanoma risk prediction tools to guide prevention and early detection advice.8 However, there was high variability among GPs in identifying melanoma risk factors and assessing how patient factors influence risk. It’s not clear from this review whether GP confidence in early detection is related to the level of prevention counselling they provide to patients.
4. New technologies to support early detection that have accompanying primary prevention advice
Five studies examined novel technologies, such as apps, to support early detection through skin examinations, which included a limited focus on providing primary preventive advice.38-42 Two of these were intervention studies using a skin self-monitoring smartphone app41 and teledermatology42 in primary care settings in the UK and Spain, respectively. Examples of primary prevention advice in these studies included personalised advice from a doctor, provision of informational pamphlets and provision of sunscreen. Both studies found high acceptability to patients and health professionals, but there was limited evidence on the benefits and cost-effectiveness of these novel approaches.
Summary of barriers and enablers to providing skin cancer primary prevention
The barriers and enablers to delivering primary prevention activities in general practice identified in the review are summarised in Table 1, mapped against the four key activities described above. Barriers and enablers were categorised according to the CFIR (Supplementary Table 2, available from: doi.org/10.6084/m9.figshare.25053656.v1), which highlighted potential influences on implementation related mainly to three domains: intervention characteristics, inner-setting and outer-setting. For example, close integration of primary prevention with routine clinical services in primary care (fit with existing workflow) was an important enabler in the inner-setting. A key enabler in the outer-setting included accessibility of risk assessment tools for patients at high risk and for the general population. We also identified some enablers that applied across various activity types, such as easy access and availability of guidelines and point-of-care tools and resources for GPs and primary care nurses to minimise disruption to flow of care. Cross-cutting barriers included competing demands and limited time within consultations, and large financial costs to deliver programs.
Table 1. Barriers and enablers to delivering skin cancer primary prevention in general practice according to activity type
| Type of activity | n (%) | Description | Implementation | ||
| Target of activity | Design of activity | Barriers | Enablers | ||
| GP knowledge, education, and training7,14–21 | 9 (29) | Practitioner | Short courses on prevention and early detection | Financial costs to deliver program | High acceptability, sharing of programs across jurisdictions |
| Patient | Campaigns for awareness, provision of information and/or invitations for skin screening | Financial costs to deliver program | Easy to understand, accessible | ||
| Behavioural counselling22-26 | 5 (16) | Practitioner | Short courses on counselling patients | Lack of standardisation on processes to deliver counselling, lack of incentives | Cost-friendly delivery, pairing with early detection |
| Patient | Direct communication with GP | Insufficient consultation times, limited availability of GP services | Easy-to-understand information | ||
| Risk assessment and delivering risk-tailored information8,27-37 | 12 (39) | Practitioner | Knowledge of risk assessment model/tools | Lack of standardisation of risk assessment processes, competing demands within consultations | Ease of access, fit with existing workflow |
| Patient | Provision of tailored risk assessment advice/materials | Lack of standardisation of risk assessment processes | High acceptability, Easy-to-understand information | ||
| Education about self-examination tools | Generalisability across populations | High feasibility | |||
| New technologies for early detection38-42 | 5 (16) | Practitioner | Use of technology and delivery of prevention advice in consults | Lack of availability of services, insufficient evidence | Fit with existing workflow |
| Patient | Use of apps for self-monitoring skin | Insufficient evidence | High acceptability, ease of access |
Discussion
This review identified four key skin cancer prevention activities that have been evaluated in primary care settings since 2011: 1) education and training programs for GPs; 2) behavioural counselling on prevention; 3) the use of novel risk assessment tools and provision of risk-tailored prevention; and 4) new technologies to support early detection that have accompanying primary prevention advice. There were a wide variety of study designs and outcomes focused on skin cancer prevention activities in primary care. They largely explored novel activities, most of which have not been implemented or translated into practice at scale.
In Australia, GPs are generally the first point of contact for patients with skin concerns.43 A large component of skin cancer–related workload involving primary prevention and dealing with patients who have suspicious symptoms or are at increased risk is dealt with in general practice.44 Although this review aimed to identify primary prevention activities in primary care settings, many of the included studies reported embedding primary prevention into strategies for early detection of skin cancer. This highlights the limited literature focused exclusively on primary prevention activities for skin cancer in primary care settings, and also aligns with the available education and training for GPs and practice nurses on skin cancer early detection, which typically includes some elements of primary prevention education.45,46
We identified enablers and barriers to delivering skin cancer prevention in primary care settings guided by framework analysis to ensure focus on delivery aspects. The review identified the main enabler to delivering primary prevention for skin cancer in primary care was to pair activities with education, training and clinical practice guidelines focused on early detection. Other research has found wide variation in approaches to integrating evidence-based knowledge for other diseases in general practice, which has implications for education and resource development.47,48 In the context of skin cancer in Australia, there may also be variation in the delivery of primary prevention activities between skin cancer-focused and other general practices.
Studies in this review showed that risk assessment tools to identify high-risk groups and provide targeted interventions show promise for improving skin cancer primary prevention and early detection in the community, which aligns with recommendations from international bodies such as the US Preventive Services Task Force (USPSTF).49 Shifts towards more risk-tailored approaches to prevention and early detection in general practice are also anticipated for other cancer types, particularly in the UK and Australia.50,51 Several web-based melanoma risk prediction tools are now available, mainly designed for health professionals to identify patients’ risk of a new or subsequent primary melanoma.
The risk assessment process provides opportunities to encourage primary prevention alongside discussions about personal risk and when to get a skin check. However, there is a need to standardise the use of these tools and the classification of ‘high risk’. Risk assessment and tailored prevention strategies should also consider how to incorporate more nuanced primary prevention messages that better incorporate the diversity of the Australian population.5 Given that some of the key barriers to delivering primary prevention activities in primary care include insufficient consultation times and competing demands on practitioners, there is a need for future research to investigate the feasibility and acceptability of fitting risk-based prevention and early detection strategies for skin cancer into models of primary care, including into health assessments offered to patients at certain ages.
The studies on novel tools and technologies identified in this review were mainly focused on supporting early detection, and incorporated limited primary prevention messages. Currently, there are apps for supporting skin cancer prevention such as the SunSmart Global UV app, which provides sun protection reminders based on reliable real-time and forecast UV levels across the world, tailored to the individual user’s location.52 This app is supported by the World Health Organization, is freely available and could be recommended to patients by their GP or practice nurse. The 2018 USPSTF evidence report and systematic review, Behavioural counselling for skin cancer prevention, found that higher-intensity interventions (for example, those that reinforced messages over time) were most likely to improve sun protection behaviours.49 A systematic review of digital interventions for promoting sun protection and skin examination behaviours has also shown promising effects, particularly for interventions that have multiple components and modalities.53 Other tools such as wearable UV sensors can be used to objectively monitor real-time personal UV exposure, which could be incorporated into primary care management for patients at high risk of skin cancer. Although UV sensors have been shown to be acceptable to patients54, these devices are not readily available and there is a need for more research examining the behavioural impact of using this type of technology within clinical care and in the community.
Limitations
Limitations of this review included that the search was limited to English language as well as to Australia and countries with comparable healthcare systems. Furthermore, this review focused exclusively on primary care. Different jurisdictions have different primary care health systems, with different models of care and funding. Therefore, findings may be less applicable to overseas juridictions.
Conclusion
Our findings can inform the development and implementation of improved skin cancer primary prevention strategies for delivery in primary care settings, to reduce the burden of skin cancer on the Australian community. Ease of program delivery, integration of preventive activities with early detection, improvements in patient awareness of skin cancer and availability of resources such as risk assessment tools are enablers to encourage and increase uptake of primary prevention behaviours in primary care, for both practitioners and patients.
Acknowledgements
AC is supported by a National Health and Medical Research Council (NHMRC) Investigator Grant #2008454. AS is supported by an NHMRC Synergy grant #2009923. KD was supported by a NHMRC Postgraduate Research Scholarship and The Eric Mather PhD Scholarship.
Peer review and provenance
Externally peer reviewed, not commissioned.
Copyright:
© 2024 Singh et al. This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International Licence, which allows others to redistribute, adapt and share this work non-commercially provided they attribute the work and any adapted version of it is distributed under the same Creative Commons licence terms.
References
- 1. Cancer Council Australia. Skin cancer incidence and morality. Skin cancer statistics and issues. Cancer Council: Sydney; 2022 [cited 2023 Dec 19]. Available from: www.cancer.org.au/about-us/policy-and-advocacy/prevention-policy/national-cancer-prevention-policy/skin-cancer-statistics-and-issues/skin-cancer-incidence-and-mortality
- 2. Gordon L, Shih S, Watts C, Goldsbury D, Green A. The economics of skin cancer prevention with implications for Australia and New Zealand: where are we now? Public Health Res Pract. 2022;32(1):31502119. CrossRef | PubMed
- 3. Shih ST, Carter R, Heward S, Sinclair C. Economic evaluation of future skin cancer prevention in Australia. Prev Med. 2017;99:7–12. CrossRef | PubMed
- 4. Montague M, Borland R, Sinclair C. Slip! Slop! Slap! and SunSmart, 1980-2000: Skin cancer control and 20 years of population-based campaigning. Health Educ Behav. 2001;28:290–305. CrossRef | PubMed
- 5. Melanoma Institute Australia and Melanoma Patients Australia. State of the nation. A report into melanoma – a national priority. Melbourne, Victoria: Insight Economics; 2022 [cited 2023 Dec 19]. Available from: melanoma.org.au/wp-content/uploads/2022/03/MIA-and-MPA_SoN-Report_Final-Report_28-March-2022.pdf
- 6. Liew AY, Cust AE. Changes in sun protection behaviours, sun exposure and shade availability among adults, children and adolescents in New South Wales, 2003-2016. Aust N Z J Public Health. 2021;45:462–8. CrossRef | PubMed
- 7. Jones S, Walker H, Maitland C. A dermoscopy training program for Victorian GPs to improve skin cancer prevention and detection. Public Health Res Pract. 2022;32(1):3212207. CrossRef | PubMed
- 8. Anandasivam B, Tam CWM, McGeechan K, Price K, McLean K, Tracy M, et al. Melanoma risk assessment and management: a qualitative study among Australian GPs. Br J Gen Pract. 2022;72:e737–46. CrossRef
- 9. Royal Australian College of General Practitioners. Guidelines for preventive activities in general practice. Melbourne, VIC: RACGP; 2018 [cited 2023 Dec 19]. Available from: www.racgp.org.au/FSDEDEV/media/documents/Clinical%20Resources/Guidelines/Red%20Book/Guidelines-for-preventive-activities-in-general-practice.pdf
- 10. Smit AK, Dunlop K, Singh N, Damian DL, Vuong K, Cust AE. Primary prevention of skin cancer in primary care settings: an Evidence Check review brokered by the Sax Institute. Sydney: Sax Institute; 2022 [cited 2023 Dec 18]. Available from: www.saxinstitute.org.au/wp-content/uploads/22.10_Evidence-Check_Primary-prevention-of-skin-cancer-in-primary-care-settings.pdf
- 11. Cooke A, Smith D, Booth A. Beyond PICO: the SPIDER tool for qualitative evidence synthesis. Qual Health Res. 2012;22(10):1435–43. CrossRef | PubMed
- 12. Hong QN, Gonzalez-Reyes A, Pluye P. Improving the usefulness of a tool for appraising the quality of qualitative, quantitative and mixed methods studies, the Mixed Methods Appraisal Tool (MMAT). J Eval Clin Pract. 2018;24(3):459–67. CrossRef | PubMed
- 13. Keith RE, Crosson JC, O’Malley AS, Cromp D, Taylor EF. Using the Consolidated Framework for Implementation Research (CFIR) to produce actionable findings: a rapid-cycle evaluation approach to improving implementation. Implement Sci. 2017;12(1):15. CrossRef | PubMed
- 14. Anders MP, Nolte S, Waldmann A, Capellaro M, Volkmer B, Greinert R, et al. The German SCREEN project – design and evaluation of the communication strategy. Eur J Public Health. 2015;25(1):150–5. CrossRef | PubMed
- 15. Bonevski B, Girgis A, Magin P, Horton G, Brozek I, Armstrong B. Prescribing sunshine: a cross-sectional survey of 500 Australian general practitioners' practices and attitudes about vitamin D. Int J Cancer. 2012;130(9):2138–45. CrossRef | PubMed
- 16. Millán-Cayetano JF, Delgado-Sánchez N, Aguilar-Bernier M, Rivas-Ruiz F, Blázquez-Sánchez N, Fernández-Canedo I, de Troya-Martín M. Skin cancer prevention: evaluation of an intervention focused on primary care. Popul Health Manag. 2019;22(3):278–9. CrossRef | PubMed
- 17. Perez M, Abisaad JA, Rojas KD, Marchetti MA, Jaimes N. Skin cancer: primary, secondary, and tertiary prevention. Part I. J Am Acad Dermatol. 2022;87(2):255–68. CrossRef | PubMed
- 18. Reeder AI Jopson JA, Gray AR. “Prescribing sunshine”: a national, cross-sectional survey of 1,089 New Zealand general practitioners regarding their sun exposure and vitamin D perceptions, and advice provided to patients. BMC Fam Pract. 2012;13:85. CrossRef | PubMed
- 19. Reinhold U, Dirschka T, Hartgens K, Kirchesch H, Ostendorf R, Petering H, et al. Vitamin D supply: from sun or pill? Attitudes and recommendation on vitamin D and impact on sun protection practices among German general practitioners evaluated by the network of dermato-oncologists, Onkoderm e.V. Oncol Lett. 2012;4(6):1392–6. CrossRef | PubMed
- 20. Rojas KD, Perez ME, Marchetti MA, Nichols AJ, Penedo FJ, Jaimes N. Skin cancer: primary, secondary, and tertiary prevention. Part II. J Am Acad Dermatol. 2022;87(2):271–88. CrossRef | PubMed
- 21. van Rijsingen MC, van Bon B, van der Wilt GJ, Lagro-Janssen AL, Gerritsen MJ. The current and future role of general practitioners in skin cancer care: an assessment of 268 general practitioners. Br J Dermatol. 2014;170(6):1366–8. CrossRef | PubMed
- 22. Hedevik H, Guorgis G, Anderson CD, Falk M. Sustainable effect of individualised sun protection advice on sun protection behaviour: a 10-year follow-up of a randomised controlled study in primary care. BJGP Open. 2019;3(3):bjgpopen19X101653. CrossRef | PubMed
- 23. Voss RK, Woods TN, Cromwell KD, Nelson KC, Cormier JN. Improving outcomes in patients with melanoma: strategies to ensure an early diagnosis. Patient Relat Outcome Meas. 2015;6:229–42. CrossRef | PubMed
- 24. Falk M, Anderson CD. Measuring sun exposure habits and sun protection behaviour using a comprehensive scoring instrument – an illustration of a possible model based on Likert scale scorings and on estimation of readiness to increase sun protection. Cancer Epidemiol. 2012;36(4):e265–9. CrossRef | PubMed
- 25. Rat C, Houd S, Gaultier A, Grimault C, Quereux G, Mercier A, et al. General practitioner management related to skin cancer prevention and screening during standard medical encounters: a French cross-sectional study based on the international classification of primary care. BMJ Open. 2017;7(1):e013033. CrossRef | PubMed
- 26. Ivers R, Jackson B, Levett T, Wallace K, Winch S. Home to health care to hospital: evaluation of a cancer care team based in Australian Aboriginal primary care. Aust J Rural Health. 2019;27(1):88–92. CrossRef | PubMed
- 27. Emery JD, Reid G, Prevost AT, Ravine D, Walter FM. Development and validation of a family history screening questionnaire in Australian primary care. Ann Fam Med. 2014;12(3):241–9. CrossRef | PubMed
- 28. Habgood E, Walter FM, O'Hare E, McIntosh J, McCormack C, Emery JD. Using an electronic self-completion tool to identify patients at increased risk of melanoma in Australian primary care. Australas J Dermatol. 2020;61(3):231–6. CrossRef | PubMed
- 29. Lophatananon A, Usher-Smith J, Campbell J, Warcaba J, Silarova B, Waters EA, et al. Development of a cancer risk prediction tool for use in the UK primary care and community settings. Cancer Prev Res (Phila). 2017; 10:421–30. CrossRef | PubMed
- 30. Quereux G, Moyse D, Lequeux Y, Jumbou O, Brocard A, Antonioli D, et al. Development of an individual score for melanoma risk. Eur J Cancer Prev. 2011;20(3):217–24. CrossRef | PubMed
- 31. Rat C, Quereux G, Riviere C, Clouet S, Senand R, Volteau C, et al. Targeted melanoma prevention intervention: a cluster randomized controlled trial. Ann Fam Med. 2014;12(1):21–8. CrossRef | PubMed
- 32. Smit AK, Newson AJ, Keogh L, Best M, Dunlop K, Vuong K, et al. GP attitudes to and expectations for providing personal genomic risk information to the public: a qualitative study. BJGP Open. 2019;3(1):bjgpopen18X101633. CrossRef | PubMed
- 33. Usher-Smith JA, Kassianos AP, Emery JD, Abel GA, Teoh Z, Hall S, et al. Identifying people at higher risk of melanoma across the U.K.: a primary-care-based electronic survey. Br J Dermatol. 2017;176(4):939–48. CrossRef | PubMed
- 34. Usher-Smith J, Emery J, Hamilton W, Griffin SJ, Walter FM. Risk prediction tools for cancer in primary care. Br J Cancer. 2015;113(12):1645–50. CrossRef | PubMed
- 35. Vuong K, Armstrong BK, McGeechan K, Cust AE. Personalized melanoma risk assessments and tailored prevention advice: a pragmatic randomized controlled trial in Australian general practice. Fam Pract. 2019;36(2):237–46. CrossRef | PubMed
- 36. Vuong K, Trevana L, Bonevski B, Armstrong B. Feasibility of a GP delivered skin cancer prevention intervention in Australia. BMC Fam Pract. 2014;15:137. CrossRef | PubMed
- 37. Falk M. Self-estimation or phototest measurement of skin UV sensitivty and its association with people’s attitudes towards sun exposure. Anticancer Res. 2014;34(2):797–803. PubMed
- 38. Jones OT, Ranmuthu CKI, Hall PN, Funston G, Walter FM. Recognising skin cancer in primary care. Adv Ther. 2020;37(1):603–16. CrossRef | PubMed
- 39. Mills K, Emery J, Lantaff R, Radford M, Pannebakker M, Hall P, et al. Protocol for the melatools skin self-monitoring trial: a phase II randomised controlled trial of an intervention for primary care patients at higher risk of melanoma. BMJ Open. 2017;7(11):e017934. CrossRef | PubMed
- 40. Nittas V, Mutsch M, Puhan MA. Preferences for sun protection with a self-monitoring app: protocol of a discrete choice experiment study. JMIR Res Protoc. 2020;9(2):e16087. CrossRef | PubMed
- 41. Walter FM, Pannebakker MM, Barclay ME, Mills K, Saunders CL, Murchie P, et al. Effect of a skin self-monitoring smartphone application on time to physician consultation among patients with possible melanoma: a phase 2 randomized clinical trial. JAMA Netw Open. 2020;3(2):e200001. CrossRef | PubMed
- 42. Milan-Cayetano J, Herrera-Ibarra R, Rivas-Ruiz F, García-Serrato P, García-Montero P, Blázquez-Sánchez N, et al. Impact of a community intervention for early skin cancer diagnosis implementing teledermatology. Acta Dermatovernerol Croat. 2020;28(2):75–9. PubMed
- 43. Baade PD, Youl PH, English DR, Elwood JM, Aitken JF. Clinical pathways to diagnose melanoma: a population-based study. Melanoma Res. 2007;17(4):243–9. CrossRef | PubMed
- 44. McAvoy BR. General practitioners and cancer control. Med J Aust. 2007;187(2):115–7. CrossRef | PubMed
- 45. University of Queensland. Master of Medicine (MMed). Brisbane: University of Queensland; 2023 [cited 2023 Dec 18]. Available from: my.uq.edu.au/programs-courses/program.html?acad_prog=5398h
- 46. McDonald S, Chong A. The prevention and early detection of skin cancer in general practice. Sydney, NSW: ThinkGP; 2023 [cited 2023 Dec 18]. Available from: www.thinkgp.com.au/education/prevention-and-early-detection-skin-cancer-general-practice-0
- 47. Le JV, Lykkegaard J, Pedersen LB, Riisgaard H, Nexøe J, Lemmergaard J, et al. Are formalised implementation activities associated with aspects of quality of care in general practice? A cross-sectional study. BJGP Open. 2017;1(2):bjgpopen17X100737. CrossRef | PubMed
- 48. Le JV, Pedersen LB, Riisgaard H, Lykkegaard J, Nexøe J, Lemmergaard J, et al. Variation in general practitioners' information-seeking behaviour – a cross-sectional study on the influence of gender, age and practice form. Scand J Prim Health Care. 2016;34(4):327–35. CrossRef | PubMed
- 49. Henrikson NB, Morrison CC, Blasi PR, Nguyen M, Shibuya KC, Patnode CD. Behavioral counseling for skin cancer prevention: evidence report and systematic review for the US Preventive Services Task Force. JAMA. 2018;319(11):1143–57. CrossRef | PubMed
- 50. Mills K, Paxton B, Walter FM, Griffin SJ, Sutton S, Usher-Smith JA. Incorporating a brief intervention for personalised cancer risk assessment to promote behaviour change into primary care: a multi-methods pilot study. BMC Public Health. 2021;21(1):205. CrossRef | PubMed
- 51. Milton S, Emery JD, Rinaldi J, Kinder J, Bickerstaffe A, Saya S, et al. Exploring a novel method for optimising the implementation of a colorectal cancer risk prediction tool into primary care: a qualitative study. Implement Sci. 2022;17(1):31. CrossRef | PubMed
- 52. Cancer Council. SunSmart App. Australia: Cancer Council; 2023 [cited 2023 Dec 19]. Available from: www.cancer.org.au/cancer-information/causes-and-prevention/sun-safety/be-sunsmart/sunsmart-app
- 53. Niu Z, Bhurosy T, Heckman CJ. Digital interventions for promoting sun protection and skin self-examination behaviors: a systematic review. Prev Med Rep. 2022;26:101709. CrossRef | PubMed
- 54. Vogel RI, Luo X, Brown K, Jewett P, Dona AC, Nagler RH, et al. A UVR-sensor wearable device intervention to reduce sun exposure in melanoma survivors: results from a randomized controlled trial. PLoS One. 2023;18(2):e0281480. CrossRef | PubMed