Abstract
Objectives: A growing number of urban development and public health professionals are developing expertise in how urban environments influence population health to support preventive health (PH) planning, implementation and outcomes. This study aimed to address the growing interest among these experts in Sydney, Australia, to move beyond silo-based approaches to PH planning and urban development by developing a preliminary mapping of the complex adaptive system. This is a network of agents and parts that collectively relate and interact, where they seek to intervene by meshing the disparate knowledge of their multidisciplinary expertise. This mapping will help experts to better integrate PH approaches by linking primordial and primary prevention within urban environments, collectively prioritising areas for intervention within the complex adaptive system, and developing a better understanding of relations between multiple factors at play within it.
Methods: The system map was developed using a unique participatory system-mapping (PSM) process involving a modified Delphi technique consisting of three rounds between October 2019 and August 2020 and 15 urban development and public health experts engaged in PH in Sydney’s urban environment.
Results: The final system map encompassed features of the local environment, determinants of health and wellbeing in urban environments, pre-clinical health and wellbeing impacts, and clinical health outcomes, providing a comprehensive map of the adverse effects of urban environments on population health. There was a high level of agreement among experts on the final system map. While experts from different disciplines generally agreed on priority areas for intervention, consensus was higher among those from similar disciplinary backgrounds.
Conclusions: The study highlights how the collective intelligence of experts from diverse disciplines can generate PSM. Furthermore, it illustrates how using systems mapping can help experts interested in complex public health problems to take a broader view of the complex adaptive system for PH planning, support collaborative prioritisation, and offer valuable insights for targeted interventions.
Full text
Introduction
Urban environments, consisting of closely related social and physical environments supporting human health and wellbeing, have become the dominant human habitat, accommodating more than half the world’s population.1 The physical environment can be subdivided into the natural environment, which consists of ecosystems such as forests and grasslands, and the built environment, including all buildings, spaces, and products created or modified by people.
There is strong evidence that urban environments affect population health1, or “the health outcomes of a group of individuals, including the distribution of such outcomes within the group”.2 Public health agencies within Australia and internationally have developed guidance cataloguing this evidence to educate professionals on how urban environments influence population health and the role of urban development in preventive health (PH).3,4 We view this as any action “aimed at reducing the likelihood that a disease or disorder will affect an individual” or group of individuals.5 This guidance recognises that urban environments provide opportunities for the implementation of both primordial prevention – targeting the wider determinants of health by addressing the environmental and social factors affecting population health – and primary prevention that focuses on shaping features within the urban environment to prevent ill-health within the population before it arises.6 Common examples include promoting active transport, access to affordable, nutritious fresh food, and decreasing risk factors for non-communicable diseases like heart disease and diabetes.
While health professionals have a crucial role in implementing PH within urban contexts, so do a range of other professions, including urban policymakers, urban planners, social planners, architects, and environmental engineers.7 Developing partnerships and intersectoral collaboration across these professions is fundamental for coordinating the planning, delivery and evaluation of PH services.8 There is a growing interest in moving beyond traditional PH approaches, which use reductionist linear cause-effect approaches as their basis.9 This interest has been attributed to the limited success of previous approaches within urban environments; these have struggled to engage with the interrelated, dynamic, and complex factors contributing to population health. These challenges are compounded by the need to bridge diverse knowledge and practices across professions.10,11 There is also interest in better understanding the complex adaptive system – a system containing many independent components that are highly connected in a non-linear and dynamic way across features of the urban environment and population health.12 The urban environment and population health form a complex adaptive system because the multiple, diverse and interacting factors and processes within urban environments simultaneously affect population health in non-linear ways.12 Understanding such systems can provide professionals with collective insight into how their PH interventions may have un/desired effects in other parts of the system. This can promote awareness of where interventions might be most beneficial.
While there has been a rise in theoretical arguments for collaborative approaches to understanding complex adaptive systems, we need more applications of these approaches to urban environments and population health in practice.13 In response, this study uses participatory system-mapping (PSM), as described by Barbrook-Johnson and Penn14, to bring together diverse disciplinary experts involved in PH across Sydney, Australia, to develop a systems map of the adverse influence of Sydney’s urban environment on population health. Systems mapping is commonly used to visualise, understand and analyse a complex adaptive system and has been applied to study diverse public health problems ranging from obesity15 to vaccine hesitancy.16 This paper contributes to systems-mapping research by describing the unique methodology developed to guide the PSM and presenting a final systems map generated by this process. We report on the study using the Standards for Reporting Qualitative Research.17
Methods
Research design
PSM comprises a set of diverse methods for visualising and analysing complex adaptive systems. We used PSM to build a preliminary visualisation of the system connecting the urban environment and population health from a multisector and multidisciplinary perspective. By meshing the mental maps of a group of experts with a wide range of backgrounds and experiences, we developed a collaborative visualisation of the system that combines the breadth and depth of expertise typically beyond the reach of individuals working alone. These experts and their knowledge of PH in Sydney formed the instrumental case study on which this mapping is based.18
Within this study, PSM takes system design tools, such as causal mapping, and embeds them in a modified Delphi process protocol to guide a group of experts through developing a map of their system. We used the Delphi process within the PSM to create an iterative approach to building consensus among the selected experts and to encourage and enable agreement across experts’ different disciplinary perspectives.19
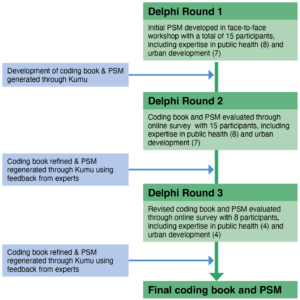
The modified Delphi technique consisted of three rounds from October 2019 to August 2020, where participants provided opinions, saw how other experts perceived these opinions, and were then allowed to amend them (see Figure 1).20 We used a 2-hour workshop as the first round of the Delphi, designed to promote engagement between experts. In contrast, the second and third rounds allowed experts to respond individually and reduce the impact of group dynamics (for example, the potential to prevent experts from speaking freely) on the resulting consensus. While the first stage of the PSM was conducted during the initial 2-hour workshop, the resulting map was further amended during stages two and three after experts provided feedback on its accuracy.
Figure 1. Methods overview (click figure to enlarge)
Note: Kumu is an online mapping tool that allows the storage of different data types behind each element and their connections
PSM = participatory system-mapping.
Expert selection and recruitment
‘Expert’ refers to urban environment and public health professionals with detailed experience researching or engaging with PH in Sydney, Australia. The research team (JP, EM), experts in both urban environments and public health, used purposive convenience sampling to develop a list of potential experts through the Maridulu Budyari Gumal: Sydney Partnership for Health, Education, Research and Enterprise (SPHERE), which includes partners from universities, local health districts, hospitals, other health networks involved in PH across Sydney. These partners include experts in urban environments, planning and development, and population health. Snowballing was then used to identify additional experts. Participants were recruited via email invitation. For the first two Delphi rounds, the workshop and the first survey, there were 15 participants, which is considered a good number for a Delphi Process in approaching PSM tasks such as this.21 For the third round, the number decreased to eight participants, largely because of the emergence of coronavirus disease 2019 (COVID-19) and increased workloads experienced by experts as they managed and responded to the pandemic.
Data collection
The initial workshop commenced with an explanation of the rules of PSM and used group techniques to elicit and mesh each expert’s tacit mental maps of the system of interest. This generated an explicit and comprehensive map with a combined breadth and depth beyond the reach of individual participants using these three steps:
- Individually, participants identified key elements within the system
- Small groups of two to three participants, combined across disciplines, created systems maps using those elements, including connections between elements
- Groups shared and linked their systems maps, adding additional elements and connections that arose during the process, and finally discussed and set boundaries for the system of interest. The combined map formed the foundation for the PSM developed through the remaining two rounds of the Delphi process.
Supplementary File A provides examples of extracts of systems maps collectively developed by experts during the initial workshop (available from: doi.org/10.6084/m9.figshare.c.6948063).
The following two rounds of the Delphi process used an online survey consisting of a series of consensus items and free-text questions requiring each expert to comment on how accurately the maps reflected the system of interest and to identify any omissions or misunderstandings. Panellists completed the two surveys over 8 months. Each survey took an average of 30 minutes and asked about:
- Primary area of expertise (public health, urban development)
- Missing elements and connections within the systems map
- Priority areas for intervention within the system map
- Level of agreement with the system map’s elements and connections
- Influence of recent significant events (e.g., COVID-19 pandemic) on their decisions.
Analysis and consensus
The first two Delphi rounds were completed and then analysed, with the results of each round informing the content for the following round, with the third Dephi round informing the content of the final codebook and map. Steps included:
Developing a code book
Using the elements and connections within the system maps drawn by experts during the initial workshop, two members of the research team from different disciplines, public health (EM) and urban planning (JP), developed an initial coding book draft using Microsoft Excel. The code book listed all elements mentioned in the systems maps and each causal link proposed by experts between those elements. The coding was guided by three principles, agreed by experts at the end of the workshop:
- All elements were grouped under four key domains: 1) features of the urban environment that can promote adverse health at the local level (e.g., buildings; 2) determinants of adverse health in urban environments (e.g., food and nutrition); 3) pre-clinical health and wellbeing impacts (e.g., psychological vulnerabilities); and 4) clinical health outcomes (e.g., diabetes)
- Elements under each key domain were grouped by subdomains to create a more manageable visualisation of the system for map users
- The connections within the map were limited to relationships that lead to adverse health and wellbeing impacts, with an endpoint of premature mortality.
These principles and the coded elements provided the boundaries that delineated the system of interest.22 Furthermore, participants asked that the mapping be presented from a macro- and micro-level perspective, as defined in the results section.
From codes to map
The collaborative systems map was generated using Kumu, a user-friendly online mapping tool that allows storing different data types behind each element and their connections.23 Once the codebook was imported into Kumu, we colour-coded the categories as per the four key domains to bring structure to the map.
Refining codes and map
The initial codebook and map were presented to the experts in round 2. Two research team members (EM, JP) used the data collected from the online survey in round 2 to revise the code book and map. The revised versions were presented to experts in round 3, and the data collected from the online survey in round 3 was used to produce the final codebook and map. The Statistical Package for the Social Sciences (SPSS) version 28 was used to analyse the survey questions.24
Ethics approval
This study was approved by the University of Technology Human Research Ethics Committee (UTS HREC REF NO. ETH21-6538).
Results
Final participatory system map
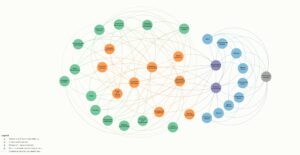
Figure 2 presents the systems map arising from the PSM. The final map was represented as a micro-level (Figure 2A) and macro-level (Figure 2B) causal process.
The micro-level causal process represents processes at the level of daily life in urban contexts. It aims to help experts tackle population health challenges in the PH system in the urban context and, ideally, to appreciate the complexity of the relationship between population health and the urban environment. The micro-level causal process encompasses urban environment features, such as inadequate housing. Additionally, it recognises the broader determinants of health and wellbeing – such as equitable access, unhealthy environmental exposures, and social exclusion – that are impacted by urban environment features. The micro-level causal process also emphasises the progression from pre-clinical health impacts, such as physical vulnerabilities, to clinical health effects like diabetes.
Figure 2A. Final participatory system map of the adverse influences of urban environments on population health for Sydney, Australia – micro-level (click figure to enlarge)
Note: the grey circle relates to premature mortality as an endpoint
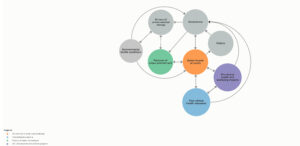
The macro-level causal process focuses on the PH system and encourages experts to consider the overarching structure underlying the system in which they operate. It comprises the key domain areas from the micro-level causal process but also includes the following system parts and their interactions: politics; governance (e.g., leadership, knowledge and data, resources, and workforce); and wider drivers of environmental change beyond the control of PH experts. Articulating the macro-level causal process helps identify where the system needs to be strengthened to support urban context-based approaches.
Figure 2B. Final participatory system map of the adverse influence of urban environments on population health for Sydney, Australia – macro-level (click figure to enlarge)
Note: the grey circles relate to the broader context of governance, politics, drivers of environmental change, and environmental health conditions
The following supplementary files further detail the system map and coding processes. Supplementary File B provides an interactive version of the systems map where the reader can zoom in. Supplementary File C provides a copy of the final coding books for features of the urban environment. Supplementary File D provides a copy of the final coding books for determinants of health and wellbeing. All supplementary files are available from: doi.org/10.6084/m9.figshare.c.6948063.
Prioritisation of areas for intervention
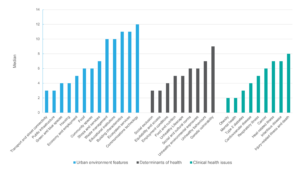
Figure 3 details the priority areas for intervention within the complex adaptive system. A lower mean indicates that more experts rated that item a higher priority, with a mean score of 2 being the highest , and a mean score of 12 being the lowest.
- For urban environment features, the areas of ‘transport and street’ connectivity and ‘public infrastructure’ were considered equally the most important priorities among all experts. Built environment experts consistently considered ‘transport and street connectivity’ the highest priority (mean 2.14), whereas health experts saw ‘housing’ (mean 3.63) as the highest priority. There was agreement across expert groups that the least important features were ‘building characteristics’, ecosystem services and ‘communications technology’.
- Under the area of social determinants of health, ‘social exclusion’ and ‘equitability and access’ were ranked equally as the highest priority among all experts. Health experts identified equitability and access as the highest priority (mean 2.75), while built environment experts identified social exclusion as the highest priority (mean 3.00).
- For clinical health issues, there was consensus that ‘obesity’ and ‘mental health’ were equally the most important priorities. Health experts rated ‘obesity’ the highest priority (mean 1.50), while built environment experts identified ‘social exclusion’ as the highest priority (mean 3.86). Both health and built environment experts viewed ‘mental health’ as an important health issue (mean 3.13, mean 2.86, respectively). They considered ‘infectious disease’ (mean 7.00, mean 6.14, respectively) and ‘injury-related illness and death’ (mean 7.88, mean 7.00, respectively) relatively insignificant.
Figure 3. Order of priorities urban environment features, determinants of health and wellbeing, as scored by experts in the final round of the Delphi procedure. (Note: A lower mean score indicates that more experts rated that item a higher priority.) (click figure to enlarge)
Level of agreement
The level of agreement among experts grew between the second and final rounds of the Delphi process. In the final round, using a scale of 1 (strongly agree) to 5 (strongly disagree):
- All participants either strongly agreed (57.1%) or somewhat agreed (42.9%) that the key elements of unhealthy urban places (features of the urban environment, determinants of health and wellbeing, clinical health outcomes) are represented in the systems model
- Most (85.7%) participants strongly agreed that the key relationships between features of the urban environment, determinants of health and wellbeing, and clinical health outcomes within the Sydney context were captured.
Influence of recent significant events
Experts were asked to what extent recent significant events, including the 2019 bushfires affecting the east coast of Australia and the emergence of COVID-19, influenced their responses during the PSM process. Most participants (60.0%) indicated that these events had little or no influence on their answers. However, 40% reported that such events influenced their perspectives to a moderate or large extent.
Discussion
In this discussion, we reflect upon key insights from the PSM process and the resulting system map.
PSM insights
While our process aligned with existing guidelines on how to conduct PSM, we tailored it to participants’ needs using a Delphi process to facilitate engagement with experts who are usually difficult to recruit due to work and time restrictions.25 We modified the Delphi by introducing an initial workshop designed to mesh the mental maps of experts with a wide range of disciplinary experience and identify system boundaries. The approach allowed the expert participants to learn about and gain experience with PSM, with participants noting that the tactile sorting of elements and connections during the workshop (using sticky notes) contributed significantly to their ability to interweave the diverse aspects of the system. Given that the use of complex systems methodology in health is in its early stages, this PSM process can be useful for the diffusion of system mapping. PSM is highly flexible and can incorporate diverse methods to suit the participant’s needs for engagement and knowledge-sharing; there is increased interest in using online workshops, although not as a substitute for face-to-face workshops.26
A second insight is that PSM enables transparent processes for developing systems maps that can increase participants’ ownership of the process. Reflecting other PSM studies, experts built the systems map during the process27 and were included in prioritising areas for intervention within the system.28 All stages of the PSM were done with participants to ensure the relevance of the map’s focus and increase participants’ ownership and commitment to the process. Experts generally noted positive outcomes from participating in the workshop stage of the PSM. This aligns with other research in which experts felt the experiences they were introduced to had helped improve coherence16 and develop knowledge29 of the broader complex adaptive systems in which they sought to intervene.
Thirdly, the PSM approach provided multiple opportunities to link back to the experts to validate the system map and prioritise areas for intervention within the system. Validation is an important step within PSM to verify data has been correctly interpreted and that no major elements have been overlooked.25 The high level of agreement reported among the experts involved in this study suggests that the PSM approach was effective at helping the multidisciplinary experts integrate their knowledge to create a collective understanding of the broader system in which they seek to intervene and then identify approaches to prioritising points for intervention within the system.
System map insights
This study’s system map intentionally “coordinate[d] expert knowledge’” of urban development and public health professionals to produce a visualisation based on their “collective intelligence” of the diverse features within the urban environment that adversely impact population health and wellbeing. At the macro-level, the map was designed to draw the attention of experts in both built environment and population health to the challenges that impact their attempts to engage in the PH system collaboratively. These factors that affect the effective operation of the PH system include knowledge/data, resourcing, and workforce. At the micro-level, the map was designed to support the development of a more synergistic response to PH by highlighting connections between “complex underlying and immediate determinants of health” on the ground.30 For example, urban development professionals’ primordial prevention approaches to features in the urban environment, such as public infrastructure, food, and housing, can be combined with primary prevention approaches by health professionals to equitable access/equity to avoid a range of adverse clinical outcomes (see Figure 2). For thinking at both the macro- and micro-level, the map complements a broader suite of tools, such as public education, legislation and regulation, community engagement, and health service orientations, that can help create more synergistic responses to PH.
A second insight related to the fact that the experts focused on harmful causal mechanisms, led to the map’s concentration on the adverse impacts of urban environments on population health. The experts were interested in developing a map that enabled them to collectively identify opportunities to disrupt or slow harmful causal mechanisms within the urban environment. They felt this focus would help them identify areas for intervention within the system – such as transport and street connectivity, housing, social exclusion, equitable access/equity, and obesity – that they believed could most effectively improve population health and wellbeing.
Limitations
Our study has several limitations, representing opportunities for further research and refinement of methods. With the emergence of COVID-19 between the various stages of the Delphi process, it was difficult to avoid experts dropping out of the research, so this incomplete participation from the sample limits the final model presented. As our focus was limited to public health and built environment experts, the perspectives of those from other sectors might have offered different and valuable perspectives on the system, and its boundaries may have been missed. Experts were purposively recruited in Sydney, so our findings may not be generalisable to other cities and regions. As this was a preliminary mapping exercise, the map produced through the PSM is relatively basic in its design; it could be redeveloped through more thorough work on causal pathways and feedback loops.
Given that this PSM aimed to develop a map based on the experts’ knowledge only, a review of peer-reviewed published literature was not used to triangulate the data on system elements. Finally, while a systems map is a static representation of a complex adaptive system, systems are constantly evolving and reorganising; as such, they need to be updated and revised regularly. Future work could revisit and refine the preliminary map, including engaging a broader range of experts and translating the prioritised areas for intervention into policy and action.
Conclusion
This study successfully developed a system map of the complex adaptive system of adverse impacts of Sydney’s urban environment on population health based on the combined knowledge of urban development and health experts. It used a unique PSM process that combined systems-thinking principles with a modified Delphi process. The PSM was shown to be an important vehicle for allowing participants to appreciate the complex adaptive system of built environment and population health. Further, it was helpful as a process for transcending disciplinary boundaries, creating a holistic visualisation of the system, and providing deeper insights into its underlying dynamics. This helped prioritise intervention points that can guide integrated PH planning. Finally, this study offers an approach that can be adopted by other multidisciplinary teams using complex systems to examine preventive health in urban environments and other contexts.
Acknowledgements
The authors would like to acknowledge the project team and funders. Investigator team: JP, EM, RL, Jon Adams, Julie Dixon, Brent Jacobs, Freya MacMillan, Andrew Gorman-Murray, Fiona Haigh, Jason De Santolo, Myna Hua, Susan Thompson, Andrew Hayen, David Sibbritt, Tina Britton, Christopher Browne, Susan Dunford, Clare Farrand, Daisy Coyle.
JP received funding for the research from the Healthy Populations and Environments Platform (formerly the Healthy Urban Environments Collaboratory), within Maridulu Budyari Gumal: Sydney Partnership for Health, Education, Research and Enterprise (SPHERE).
This paper is part of a special journal issue focusing on urban planning and development for health, which has been produced in partnership with the Healthy Populations and Environments Platform, SPHERE. JP was a guest editor for the special issue but was not involved in the review of or decisions on this manuscript.
Peer review and provenance
Externally peer reviewed, invited.
Copyright:
© 2023 Prior et al. This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International Licence, which allows others to redistribute, adapt and share this work non-commercially provided they attribute the work and any adapted version of it is distributed under the same Creative Commons licence terms.
References
- 1. Capon A. Harnessing urbanisation for human wellbeing and planetary health. Lancet Planet Health. 2017;1(1):e6–e7. CrossRef | PubMed
- 2. Kindig D, Stoddart G. What is population health? Am J Public Health. 2003;93(3):380–3. CrossRef | PubMed
- 3 . NSW Health, Healthy urban development checklist: a guide for health services when commenting on development policies, plans and proposals. Sydney: NSW Health; 2009 [cited 2023 Nov 20]. Available from: www.parliament.nsw.gov.au/lcdocs/other/10375/Answers%20to%20questions%20on%20notice%20-%20NSW%20Health%20-%20Att%202.PDF
- 4. Public Health England. Spatial planning for health: an evidence resource for planning and designing healthier places. UK: Public Health England; 2017 [cited 2023 Nov 20]. Available from: assets.publishing.service.gov.uk/media/5b59b090e5274a3ff828c70c/spatial_planning_for_health.pdf
- 5. World Health Organization. WHO global forum IV on chronic disease prevention and control. Geneva: WHO; 2004 [cited 2023 Nov 20]. Available from: apps.who.int/iris/bitstream/handle/10665/43208/9241593164_eng.pdf
- 6. Australian Government Department of Health and Aged Care. National preventive health strategy 2021–2030. Canberra: Australian Government; 2021 [cited 2023 Nov 20]. Available from: www.health.gov.au/resources/publications/national-preventive-health-strategy-2021-2030?language=en
- 7. Prior J, Connon I, McIntyre E, Adams J, Capon A, Kent , et al. Built environment interventions for human and planetary health: integrating health in climate change adaptation and mitigation. Public Health Res Pract. 2018;28(4);e2841831. CrossRef | PubMed
- 8. World Health Organization. Rio political declaration on social determinants of health. Geneva: WHO; 2011 [cited 2023 Nov 20] Available from: www.who.int/publications/m/item/rio-political-declaration-on-social-determinants-of-health
- 9. Lawrence RJ, Gatzweiler FW. Wanted: a transdisciplinary knowledge domain for urban health. J Urban Health. 2017;94(4):592–6. CrossRef | PubMed
- 10. Lawrence RJ. Creating built environments: bridging knowledge and practice divides. New York, New York: Routledge; 2021. CrossRef
- 11. Collyer TA, Smith KE. An atlas of health inequalities and health disparities research: “How is this all getting done in silos, and why?”. Soc Sci Med. 2020;264:113330. CrossRef | PubMed
- 12. Gatzweiler FW, Reis S, Zhang Y, Jayasinghe S. Lessons from complexity science for urban health and well-being. Cities & Health. 2017;1(2):210–23. CrossRef
- 13. Muñoz-Erickson TA, Miller CA, Miller TR. How cities think: knowledge co-production for urban sustainability and resilience. Forests. 2017;8(6):203. CrossRef
- 14. Barbrook-Johnson, P, Penn AS. (2022). Participatory systems mapping. In: Systems mapping: how to build and use causal models of systems (pp. 61-78). Cham: Springer International Publishing. CrossRef
- 15. UK Government’s Foresight Programme. Reducing obesity: obesity system map. UK: Government Office for Science; 2007 [cited 2023 Nov 20]. Available from: www.gov.uk/government/publications/reducing-obesity-obesity-system-map
- 16. Decouttere C, Banzimana S, Davidsen P, Van Riet C, Vandermeulen C, Mason E, et al. Insights into vaccine hesitancy from systems thinking, Rwanda. Bull World Health Organ. 2021;99(11):783–94D. CrossRef | PubMed
- 17. O’Brien BC, Harris IB, Beckman TJ, Reed DA, Cook DA. Standards for reporting qualitative research: a synthesis of recommendations. Acad Med. 2014;89(9):1245–51. CrossRef | PubMed
- 18. Crowe S, Cresswell K, Robertson A, Huby G, Avery A, Sheikh A. The case study approach. BMC Med Res Methodol. 2011;11(1):100. CrossRef | PubMed
- 19. Ratnapradipa D, Brown SL, Wodika AB. Examining the breadth and depth of environmental health through a modified Delphi technique. American Journal of Health Education. 2011;42(1):50–7. CrossRef
- 20. Massaroli A, Martini JG, Lino MM, Spenassato D, Massaroli R. Método delphi como referencial metodológico para a pesquisa em enfermagem. [The Delphi method as a methodological framework for research in nursing]. Texto & Contexto-Enfermagem. 2018:26(4):e1110017. CrossRef
- 21. Manoliadis O, Tsolas I, Nakou A. Sustainable construction and drivers of change in Greece: a Delphi study. Construction Management and Economics. 2006;24(2):113. CrossRef
- 22. Plsek PE, Greenhalgh T. The challenge of complexity in health care. BMJ. 2001;323:625–8. CrossRef | PubMed
- 23. Mohr J, Mohr R. Kumu - Relationship Mapping Software. 2019 [cited 2023 Nov 20]. Available from: kumu.io.
- 24. IBM Corp. IBM SPSS Statistics for Windows, Version 28.0. IBM Corp. Armonk, NY; 2021 [cited 2023 Nov 20]. Available from: www.ibm.com/products/spss-statistics
- 25. Barbrook-Johnson P, Penn AS. What data and evidence can you build system maps from? In: Barbrook-Johnson P, Penn AS, editors. Systems mapping: how to build and use causal models of systems. Cham: Springer International Publishing; 2022. pp. 129–43. CrossRef
- 26. Chavez-Ugalde Y, Toumpakari Z, White M, De Vocht F, Jago R. Using group model building to frame the commercial determinants of dietary behaviour in adolescence - proposed methods for online system mapping workshops. BMC Med Res Methodol. 2022;22(1):84. CrossRef | PubMed
- 27. Ansah JP, Islam AM, Koh V, Ly V, Kol H, Matchar DB, et al. Systems modelling as an approach for understanding and building consensus on non-communicable diseases (NCD) management in Cambodia. BMC Health Serv Res. 2019;19(1):2. CrossRef | PubMed
- 28. Mui Y, Ballard E, Lopatin E, Thornton RLJ, Pollack Porter KM, Gittelsohn J. A community-based system dynamics approach suggests solutions for improving healthy food access in a low-income urban environment. PLoS One. 2019;14(5):e0216985. CrossRef | PubMed
- 29. Atkinson J-A, Wells R, Page A, Dominello A, Haines M, Wilson A. Applications of system dynamics modelling to support health policy. Public Health Res Pract. 2015;25(3);e2531531. CrossRef | PubMed
- 30. Nutbeam D. Promoting health, preventing disease – making it happen. Public Health Res Pract. 2019;29(4):e2941930. CrossRef | PubMed