Abstract
Consumer and community involvement (CCI) in preventive research and health initiatives is not only encouraged but is expected within a rapidly evolving landscape across health policy, practice and research. Here, we summarise the fundamental principles of CCI, as well as outline the barriers and current developments in working towards best practices at organisational and systems levels. CCI stands at a critical juncture. Best practice emphasises meaningful partnerships with consumers and communities to deliver impactful research and prevention activities, yet complex challenges and systematic barriers remain. We need further evidence to demonstrate both ‘what’ and ‘how’ CCI should be best implemented in these settings. We present key considerations for researchers, organisations and systems to catalyse the transition of CCI from mere recognition of its importance to pragmatic and optimum implementation and, ultimately, to systemic reform. These include changes to capacity building, funding structures, equitable engagement and transparent evaluation. These must be underpinned by evidence-based approaches, partnership, trust and broad consensus processes to achieve meaningful and impactful CCI in research and healthcare improvement through a lens of inclusivity.
Full text
Consumer and community involvement: an introduction
In the context of a growing global crisis in managing the burden of non-communicable diseases (NCDs), there is increased urgency to focus on public health prevention measures. This is emphasised in current national preventive health strategies in Australia1, the US, the UK and elsewhere.2-4 These strategies are supported by the significant return on investment of public health interventions and measures in low-, low- to middle-, and high-income countries, where typically, the broader the intervention reach, the greater the return on investment. As such, consumer and community involvement (CCI) and partnership in initiatives to improve health are now not only encouraged but expected, to ensure that the real-world values, needs and preferences of increasingly diverse communities are met.5,6 CCI is complex, with evolving and inconsistent terminology and overarching concepts7, and a lack of recognition of CCI as not only a process but an outcome. CCI is commonly defined as consumers and communities actively working with researchers or organisations to help shape decisions that are made with or by consumers and their communities, rather than for them.8 Frameworks for CCI are frequently underpinned by equity, fostering of trust and partnerships, opportunities for development, evaluation, and transparent processes and governance. Such frameworks also typically recognise the broad nature of engagement that varies according to the type of required activity and availability of resources. The International Association for Public Participations’ (IAP2) Spectrum which spans informing, consulting, involving, collaborating and empowering is often cited as a framework for CCI.9 In preventive health research, common CCI activities include shaping research questions, optimising design and methodologies and translating research outcomes that are relevant for end-users, with a community-centric focus. Consumers’ lived experiences, coupled with cultural nuances, are considered equally important and complementary to the professional knowledge and skills contributed by researchers and other stakeholders. The incorporation of diverse contributions aims to enhance overall effectiveness and inclusivity, guiding the development of effective, ethical, and community-centric initiatives in preventive and public health.10
Current insights and barriers to best practice CCI
Australia’s National Preventive Health Strategy 2021–2030 calls for the active use of community prevention partnerships to build capacity and practice change for better health outcomes1 To guide the implementation of this vision, the National Consumer Engagement Strategy for Health and Wellbeing has been drafted11, advocating multidimensional engagement strategies that build trust in partnership, enhance the capability of those responsible for engagement and empower consumers to engage in co-design approaches that are equitable and effective. The Engagement Strategy proposes good practice guidelines for consumer engagement with an accompanying toolkit of factsheets and checklists to assist users in its implementation.
Likewise, national governing bodies for research, including the Australian National Health and Medical Research Council (NHMRC) and accredited Research Translation Centres within the Australia Health Research Alliance (AHRA) have undertaken commendable efforts to foster a shared vision, consistent terminology, and standardised processes for CCI.12,13The NHMRC collaborated with the Consumers Health Forum of Australia to release a statement on CCI in 201612 and is currently undertaking national consultation to update this statement to reflect recent progress. The Australian Medical Research Future Fund (MRFF) also emphasises consumers leading and guiding all research it funds, including adopting principles for consumer involvement and establishing a Consumer Reference Panel to provide advice on strategies for strengthening CCI.14
Despite these advancements in CCI, critical barriers remain in its implementation at organisational and systems levels. These include: a lack of capacity, practical knowledge and resourcing; use of inconsistent terminology; conflicting attitudes disciplinary, political and philosophical perspectives towards CCI; and an absence of embedded, on-the-ground processes to guide ‘what’ and ‘how’ to best implement CCI. Ensuring CCI is not tokenistic is crucial. At present, not every voice is equally heard, and marginalised and underrepresented communities often face exclusion or poorly executed inclusion efforts. Superficial efforts occur where institutions present an image of inclusivity without implementing the necessary methods, mechanisms, and ethical frameworks that uphold the principles of genuine, diverse engagement.15 Such efforts can occur when health literacy levels are met. Therefore, individuals may be excluded from technical discussions, avoid passivity in decision-making, recognition of the value of lived experience and appropriate remuneration provisions. Continuous research into and evaluation of how CCI is implemented to ensure its relevance and effectiveness is important, particularly in the context of addressing the global health challenge posed by non-communicable diseases.10
Moving towards meaningful CCI: key considerations
The urgency to drive change across preventive health research structures, policies, practices and evaluation methods to ensure best practice CCI is evident. We look forward to the further development of practical evidence about ‘what’ and ‘how ’ to implement best practice CCI at organisation- and system-levels. This will inform the vision, principles and frameworks, training resources and national statements, including those described above.
Key considerations for researchers and stakeholders for best-practice CCI include:
1. Build capacity in CCI
In Australia, research bodies including the Australian Health Research Alliance, NHMRC, MRFF, Australian Clinical Trials Alliance and the Collaboration for Enhanced Research Impact (CERI) NHMRC Centres of Research Excellence are actively shaping the evolution of CCI. We advocate national partnerships, implementation research and collective knowledge-sharing to underpin and progress towards implementation of best practice CCI in research.
By 2030, the National Preventive Health Strategy 2021–2030 aims to establish a widely accessible mechanism for enhancing the sharing of information on best practice interventions.1 At the time of writing, a national interactive, digital CCI knowledge hub is under development by AHRA and CCI partners, with broad consumer engagement to provide consistent messaging, knowledge, evidence-based tools and resources, support for best practice approaches and examples of CCI for advancing knowledge and building capacity.12 This, and other efforts as part of the AHRA CCI initiative, are expanding insights into both the ‘what’ and ‘how’ in CCI. This includes enabling all stakeholders to navigate best inclusive and equitable practices and facilitating more sophisticated integration and meaningful CCI to produce significant outputs for preventive health research, practice, and policy domains and benefits for end-users.
2. Funding for embedded CCI within research and healthcare programs
While best practice guidance by key Australian funding bodies encourages CCI in health and medical research and there have been changes to key assessment criteria, it is not currently a mandated requirement of key Australian grant funding bodies.14 Similarly, while both the UK and US recognise the importance of patient involvement in health research, it is merely encouraged, and not a requirement for grant funding.2-4 Recent surveys of researchers and clinical trial networks reported that 50% of clinical and primary care trials and up to 75% of pragmatic trials include CCI, where involvement in study protocol development is the most commonly cited activity, followed by intervention design and participant retention strategies demonstrating similar international situations for CCI.16-18 Frequently, studies revealed discrepancies between planned and actual CCI activities, with only a minority providing published methodology and outcomes.16-18 Moreover, limited use of a structured CCI process and minimal provision of CCI training to researchers or facilitators has been reported, leading to uncertainty regarding the quality of CCI undertaken16-18.To address these issues, we suggest that researchers should include a dedicated budget for CCI in research projects and/or request specific funding for it in funding proposals. This will assist in planning CCI activities and enable forecasting of resources and capacity-building requirements from the outset. Increased funding for consumer remuneration for involvement in studies may also facilitate better uptake of CCI, as remuneration has been shown to build respect and trust and facilitate equitable engagement with consumers.19 With CCI activities increasingly part of research funding assessment criteria, this too will propel rigour in CCI engagement activities and enhance transparency in reporting of outcomes.
3. Ensure equity and cultivate diversity
While CCI is universally important, it is particularly crucial in priority populations, where a disproportionate burden of disease exists.1,20 This higher burden of disease is often rooted in social inequality and disadvantage that would benefit from preventive health initiatives. Globally, while these groups share similarities, specific priority populations vary. In Australia, priority groups include Aboriginal and Torres Strait Islander peoples (First Nations or Indigenous); culturally and linguistically diverse people; lesbian, gay, bisexual, transgender, queer or questioning, and other identities (LGBTQI+) individuals; those with mental illness, low socioeconomic status; and those living with disability and/or in rural, regional, and remote areas.
Proactively tackling societal and health-related stigma and discrimination is essential for fostering a supportive environment that is conducive to participation and collaboration. It is important to provide robust support for individuals involved in CCI initiatives to ensure diverse community perspectives are represented in projects or committees. This includes providing proper orientation and support for consumers into projects, and active involvement in understanding and directing the outcomes and evaluation, including accommodating additional needs where required to enable active contribution to discussions.
Dismantling prejudices and biases within CCI initiatives empowers individuals and fosters authentic collaboration. This involves dedicating time and resources to engaging with community leaders, reducing stigma, fear, and discrimination against those with lived experiences. Building relationships within a CCI group can offer rich perspectives. Fostering inclusivity values diverse voices which recognises varying levels of health literacy, and recognises the need for adequate resourcing for effective implementation.
4. Transparency in evaluation for shared learnings and continuous improvement
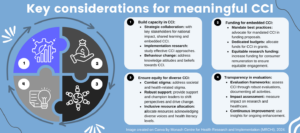
The addition of evaluation that measures impact and allows for continuous improvement to current CCI frameworks is fundamental. Assessing and documenting the effectiveness of CCI through evaluation of what activities occurred, process measures, deviations, how CCI was implemented and associated budget will enable shared learnings in CCI. Organisations and systems can then allocate resources strategically and plan initiatives that genuinely contribute to positive outcomes in preventive research. Similar to broader concepts of CCI, effective evaluation also necessitates robust collaborations with consumers and communities. This approach ensures ethical, responsive, and beneficial evaluations that align with the needs and priorities of end-users A graphic representation of key considerations is shown in Figure 1.
Figure 1. Key considerations for consumer and community involvement (CCI) (click figure to enlarge)
Conclusion
The evolution of CCI in preventive health research has progressed from acknowledging its importance to advocating its best-practice implementation. Australia’s national health strategies emphasise community-centric preventive health initiatives, ensuring relevance and equity. The research landscape supporting prevention is rapidly evolving, with national policies and partnerships emphasising meaningful CCI. It is vital to embrace best-practice CCI to achieve effective prevention research and practice. There now needs to be a focus on evolving policies, frameworks, and large-scale activities, to emphasise a shared vision, evidence-based processes and systems-level approaches to CCI. This encompasses the need for a genuine sharing of power, mutual trust, and a shared belief in the value of CCI. This will require the leveraging of partnerships and collaboration, policy and funding mechanisms and access to resources to deliver mutual impact in preventive health research and actions alike, to ultimately deliver better and more equitable health outcomes.
Acknowledgements
This paper is part of a special issue of the journal focusing on: ‘Collaborative partnerships for prevention: health determinants, systems and impact’. The issue has been produced in partnership with the Collaboration for Enhanced Research Impact (CERI), a joint initiative between The Australian Prevention Partnership Centre and NHMRC Centres of Research Excellence. The Prevention Centre is managed by the Sax Institute in collaboration with its funding partners.
CH was a guest editor for the special issue. She had no involvement in the review of or decisions on this manuscript.
Peer review and provenance
Externally peer reviewed, invited.
Copyright:
© 2024 Brammall et al. This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International Licence, which allows others to redistribute, adapt and share this work non-commercially provided they attribute the work and any adapted version of it is distributed under the same Creative Commons licence terms.
References
- 1. Department of Health and Aged Care, Australia. National Preventive Health Strategy 2021–2030. Canberra: Australian Government; 2021 [cited 2024 Feb 23]. Available from: www.health.gov.au/resources/publications/national-preventive-health-strategy-2021-2030?language=en
- 2. Frank L, Basch E, Selby JV, Institute P-COR. The PCORI perspective on patient-centered outcomes research. JAMA. 2014;312(15):1513–14. CrossRef | PubMed
- 3. National Institute for Health and Care Research. PPI (Patient and Public Involvement) resources for applicants to NIHR research programmes. US; NIHR; 2019. [cited 2024 Mar 04]. Available from: www.nihr.ac.uk/documents/ppi-patient-and-public-involvement-resources-for-applicants-to-nihr-research-programmes/23437
- 4. National Institute of Health and Care Excellence. Patient and public involvement policy. UK: NICE; 2024 [cited 2024 Mar 4]. Available from: www.nice.org.uk/about/nice-communities/nice-and-the-public/public-involvement/public-involvement-programme/patient-public-involvement-policy
- 5. Greenhalgh T, Hinton L, Finlay T, Macfarlane A, Fahy N, Clyde B, et al. Frameworks for supporting patient and public involvement in research: systematic review and co‐design pilot. Health Expect. 2019;22(4):785–801. CrossRef | PubMed
- 6. Reeder S, Ayton D, Teede HJ, Skouteris H, Simmons M, Jones A. Opportunities to enhance consumer and community engagement training for researchers and healthcare providers: a qualitative study. BMJ Open. 2023;13(9):e073114. CrossRef | PubMed
- 7. Israel BA, Schulz AJ, Parker EA, Becker AB. Critical issues in developing and following community-based participatory research principles. Community-based participatory research for health. San Francisco, CA, Jossey-Bass, 2008. pp. 47–62.
- 8. Monash Partners. Platforms. Consumer and Community Involvement. Melbourne: Monash Partners; 2024 [cited 2024 Mar 4]. Available from: monashpartners.org.au/disciplines/consumer-and-community/
- 9. IAP2 Australasia. IAP2 Public Participation Spectrum. Queensland: IPA2; 2019 [cited 2024 Mar 4]. Available from: iap2.org.au/resources/spectrum/
- 10. Barone MTU, Klatman E. Meaningful engagement of people living with noncommunicable diseases: challenges and opportunities. J Patient Experience. 2024;11:23743735231224560. CrossRef | PubMed
- 11. Department of Health and Aged Care, Australia. Draft national consumer engagement strategy for health and wellbeing. Canberra: Australian Government; 2023 [cited 2023 Nov 23]. Available from: consultations.health.gov.au/national-preventive-health-taskforce/draft-national-consumer-engagement-strategy-for-he/supporting_documents/Draft%20National%20Consumer%20Engagement%20Strategy%20for%20Health%20%20Wellbeing%20NCESHW.pdf
- 12. Australian Health Research Alliance. Consumer and community involvement. Western Australia; AHRA; 2023 [cited 2023 Sep 21]. Available from: ahra.org.au/our-work/consumer-and-community-involvement
- 13. National Health and Medical Research Council. Statement on consumer and community involvement in health and medical research. Consumers Health Forum of Australia. Canberra: NHMRC; 2016 [cited 2024 Mar 2]. Available from: www.nhmrc.gov.au/about-us/publications/statement-consumer-and-community-involvement-health-and-medical-research
- 14. Department of Health and Aged Care. Principles for consumer involvement in research funded by the Medical Research Future Fund. Canberra: Australian Government; 2023 [cited 2023 Nov 23]. Available from: www.health.gov.au/resources/publications/principles-for-consumer-involvement-in-research-funded-by-the-medical-research-future-fund?language=en
- 15. Majid U. The dimensions of tokenism in patient and family engagement: a concept analysis of the literature. J Patient Experience. 2020;7(6):1610–20. CrossRef | PubMed
- 16. McKenzie A, Bowden J, Zalcberg JR, Conroy K, Fallon-Ferguson J, Shilpanjuali J et al. A snapshot of consumer engagement in clinical trials in Australia: results of a national survey of clinical trial networks and research organisations. Res Involv Engagem. 2022;8(1):3. CrossRef | PubMed
- 17. Vanderhout S, Nevins P, Nicholls SG, Macarthur C, Brehaut C, Potter BK et al. Patient and public involvement in pragmatic trials: online survey of corresponding authors of published trials. CMAJ Open. 2023;11(5):E826-37. CrossRef | PubMed
- 18. Blackburn S, McLachlan S, Jowett S, Kinghorn P, Gill P, Higginbottom A et al. The extent, quality and impact of patient and public involvement in primary care research: a mixed methods study. Res Involv Engagem. 2018;4:16. CrossRef | PubMed
- 19. Richards DP, Cobey KD, Proulx L, Dawson S, de Wit M, Toupin-April K. Identifying potential barriers and solutions to patient partner compensation (payment) in research. Res Involv Engagem. 2022;8(1):7. CrossRef | PubMed
- 20. Australian Institute of Health and Welfare. Australian Burden of Disease Study: impact and causes of illness and death in Australia 2015. Canberra: AIHW; 2019.[cited 2024 Mar 3]. Available from: www.aihw.gov.au/reports/burden-of-disease/burden-disease-study-illness-death-2015/summary