Abstract
Objectives: While systems thinking has gained recognition as an important approach in health policy and prevention research, its application in the context of fall prevention among community-dwelling older adults has been underutilised. Here, we build on the guiding principles of the systemic lens component of the Prevention System Change Framework to assess and identify potential changes that are required to facilitate policy action in the field of falls prevention.
Methods: We conducted a desktop search to identify policy documents encompassing falls prevention among community-dwelling older adults in Australia. Documents were considered eligible if they were published in the last 10 years and were authored or endorsed by federal or state government bodies. We collaboratively examined eligible documents to gain insights into the current policy landscape in falls prevention and to illustrate opportunities for action and the potential for strengthening partnerships.
Results: There is no current national policy on preventing falls in older adults in Australia. While we identified eight policy documents, none focused exclusively on falls prevention, indicating that falls are currently not perceived as a public health issue that warrants a dedicated policy framework. We identified a need for a comprehensive national policy that draws upon insights from various disciplines, suggests intersectoral collaboration, addresses health inequities and involves meaningful engagement with key stakeholders. Future falls prevention policies may benefit from clear governance structures and specific targets, along with mechanisms for monitoring and evaluating outcomes.
Conclusion: Falls prevention is a pressing public health concern that requires dedicated policy resources. Adopting a systems-oriented approach can help reduce falls and their associated burdens on individuals and the healthcare system. Acknowledging the urgency and complexity of this challenge is a first, essential step toward crafting a comprehensive national falls prevention policy.
Full text
Introduction
Falls have substantial consequences for older Australians, presenting both individual and systemic challenges. At the individual level, falls can lead to injuries, negative emotions and concerns about future falls, leading to increased dependency and reduced overall quality of life.1 At their worst, falls can be fatal, with older Australian adults (65 years and older) being 68 times more likely to die from a fall than individuals aged 15–64 years.2 At the healthcare system level, falls are the leading cause of injury-related deaths across all age groups, disproportionately impacting older adults, who account for 94% of all fall-related deaths.2 Alongside the burden on individuals and the healthcare system is the financial impact – it is estimated that falls in individuals aged 65 years and older cost the Australian healthcare system A$2.3 billion each year.2
Despite these alarming statistics, which are similar to those of other countries, falls have not garnered sufficient policy attention as a public health issue in Australia, or elsewhere, as highlighted by the World Health Organization (WHO).3 Currently, there are no frameworks that consider or examine the multifaceted nature of falls, influenced by individual, familial, environmental, societal, political, cultural, and healthcare-system factors. To address this, we propose a shift towards system-oriented research alongside clinical and healthcare system research. This approach aligns with growing calls from policymakers, health professionals and researchers for more system-oriented analyses and actionable solutions to address public health challenges.4
Systems thinking has been highlighted as an effective approach to understanding and proposing actions on many complex public health challenges such as tobacco smoking5 and obesity.6 By definition, systems thinking is a way to make sense of a complex issue and improve problem-solving by uncovering connected and interrelated components, offering important insights into the relationships, boundaries and perspectives within a system.7 A key approach to systems thinking is to apply a system lens to understand an existing policy landscape by analysing the content of policy documents to understand how the problem is framed, along with proposed solutions and involved stakeholders.8 This approach can be useful to promote ‘policy learning’, allowing for adaptation, identifying gaps and gaining insights into the conditions necessary for a policy to be successful.9
In this study, we use the first component of the Prevention Systems Change Framework (PSCF)10, which investigates the policy landscape, to analyse the current landscape of Australian fall-prevention policies.10 The PSCF was developed by systems-thinking researchers to provide a pathway for systems change through reflective learning, followed by the development and implementation of the theory of systems change. The PSCF prompts prevention researchers to move beyond describing systems and advocates for action-oriented research. This is facilitated by guiding systems-based research planning, monitoring and study team reflective learning through four iterative steps in prevention research: 1) applying a system lens to the prevention problem being studied; 2) adopting an implementation focus; 3) integrating the systems lens and the implementation focus; and 4) developing a theory of systems change.10 Given the extensive range of methods and stakeholders that are necessary to thoroughly address PSCF components 2 to 4, we focused on the first component only in this study.
The work is part of a broader effort aimed at reinforcing advocacy and interdisciplinary work in falls prevention.11 Guided by the PSCF, we examined national and state Australian policy documents to promote falls prevention in Australia. We aimed to understand the current landscape of policies targeting falls prevention and identify potential pathways for change. To achieve this, we have asked the following questions: 1) what content do falls prevention policies cover? and 2) what are the gaps in the current policy landscape, and how can they be addressed to improve falls prevention?
Methods
Firstly, we conducted a content analysis of falls-related policy documents using two strategies to identify them: 1) a comprehensive desktop search conducted by NC, MA and two research assistants in June 2022 and repeated in September 2023 (see search strategy in Supplementary file 1, available from: doi.org/10.6084/m9.figshare.25241818); and 2) reviewing policy documents already known to the team. Policy documents were considered eligible if they met the following five criteria: were publicly available; referenced falls within the context of older adults; included a “broad statement of goals, objectives and means that create the framework for activity”12; were published in the past 10 years; and were commissioned, produced or endorsed by federal or state government authorities. All identified documents were screened by two reviewers and included documents were analysed using content analysis. To this end, NC read and re-read all included documents to get a sense of the whole and imported them into NVivo 14 software (Melbourne, Australia; QSR International; NVivo, 2023) for manual coding, which involved grouping excerpts of texts into codes and categories. MA double-checked codes and themes and made suggestions to refine those. A summary of the content analysis was shared with co-authors for review.
Secondly, to further assist the interpretation of the content analysis and examine the systemic context of falls prevention efforts, the authors collaboratively examined the policies over two 2-hour meetings, guided by the PSCF component 1 questions (‘Applying a system lens’) (see Supplementary file 2, available from: doi.org/10.6084/m9.figshare.25241821). We used excerpts of the policy documents as prompts (see Supplementary file 3, available from: doi.org/10.6084/m9.figshare.25241824) while also considering our combined expertise and experiences in falls prevention research, public health, health policy, urban planning, aged care, health economics, housing, health inequities and advocacy for policy change. The two collaborative discussions were audio-recorded and the main discussion points from each meeting were summarised by NC, who shared the analytic summaries with the team for further input. NC also re-read the eight included policy documents, codes and themes to further elaborate on the points raised during the team analysis. The outcomes of both the content analysis and these collaborative discussions are presented below as a narrative synthesis, structured around the six domains of the PSCFs ‘applying system lens’ component, namely: policies; connections and boundaries; power and control dynamics; system regulations; values and norms; and system interdependencies.
This study was funded by the National Health and Medical Research Council (NHMRC) Centre for Research Excellence (CRE) in the Prevention of Falls Injuries.
Results
In the content analysis, we assessed 47 documents for eligibility, out of which eight were selected for detailed analysis (see Supplementary file 4, available from: doi.org/10.6084/m9.figshare.25241830).13-20 The themes and subthemes identified are presented below (see Supplementary file 3 for excerpts, available from: doi.org/10.6084/m9.figshare.25241824).
Description of falls
Most documents discussed falls by mentioning epidemiological data13,14,16-18 and/or discussed risk factors for falls.13-16,18 Falls were highlighted as burdensome and associated with poor nutrition, physical inactivity, chronic diseases and an increased likelihood of being admitted to aged care facilities. Notably, some documents identified gaps in the literature, such as the cost-effectiveness of balance programs in rural/remote areas14, and in service provision (for example, limited assessment and intervention for falls).18
Goals
All documents presented health-related goals, and most presented goals specific to falls, with one exception.13 Fall-related goals included: reducing falls; preventing falls; decreasing the impact of falls (e.g., decreasing the proportion of older people with fall-related insecurities); supporting an online directory of community-based physical activity and fall prevention; delivering a free falls prevention program (Stepping On); expanding falls prevention programs in regional areas; establishing education programs targeting falls; expanding emergency department falls services; and working with stakeholders to develop a strategic action plan for falls. While the National Preventive Health Strategy 2021–203013 did not state any specific goals related to falls, it discussed how improving access to and the consumption of a healthy diet and increasing physical activity can reduce falls; we considered it eligible for inclusion as it broadly provided a framework for reducing falls.
Collaborations
All but one policy document highlighted the contributions of several stakeholders to the document’s development. However, the collaboration was not always described in detail. For instance, only two documents stated that the priorities were identified in consultation with stakeholders19.20 and only two provided a detailed description of how the consultation with stakeholders took place.14,20 Most documents elaborated on the importance of meaningful collaborations to achieve desired goals13,14,16-18,20 but few emphasised the importance of collaboration across sectors.13,16,20
Actions targeting falls
All documents but one described action to be undertaken to achieve desired goals. Examples include, but are not limited to: improving access to home environment assessment and modification opportunities; increasing access to falls prevention programs; including culturally relevant programs; including design features to reduce falls in public buildings and paths (e.g., National Injury Prevention Strategy 2020–203014) and ensuring that health services organisations have guidelines and models of care for falls prevention (e.g., The National Safety and Quality Health Service (NSQHS) Standards15).
Monitoring and reporting
While most documents highlighted the importance of monitoring and reporting, only half specifically named indicators that could be considered within the context of falls prevention (for example, rate of falls; years of life lost due to falls; number of hospitals with pathways to address falls; fall-related injury hospitalisations among people aged 65 and older; and confidence to live independently with fewer falls-related insecurities).14,15,17,20
Key Stakeholders
Key stakeholders were mentioned in all documents, although varied substantially – from unidimensional and individual-focused (e.g., clinicians, families)15 to cross-sectoral, including academics, all governments, business sector, communities, families, healthcare systems, individuals, industry, private health insurers, nongovernment organisations and others.13
Analysis and discussion
We have combined the results of our collaborative analysis drawing from the questions posed by the PSCF and our discussion in the section below, with a view to presenting our interpretative analysis alongside the broader context of the literature.
Applying a system lens for falls prevention
Policies: What gaps in policy exist to build the system? What additional policies and programs are needed?
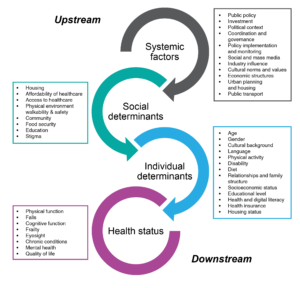
Our analysis of falls prevention policies identified the need for a comprehensive national policy dedicated to falls prevention. Such a policy should acknowledge the multidimensional nature of the problem and call for multisectoral action, beyond government departments and agencies. For instance, although the draft National Injury Prevention Strategy 2020–203014 covers important factors that impact falls, such as housing standards and exercise programs, other relevant factors, such as nutrition and public awareness, are not mentioned. Notably, none of the reviewed policy documents covered all the necessary factors that may be relevant for falls prevention policy as informed by systems thinking (Figure 1). Additionally, the policy documents generally lacked clarity regarding how strategies would be implemented, outcomes monitored and evaluated, and governance structures (who will do what, when, where and why), although there were two exceptions in which some of these aspects were clearer.17,20 At times, the fall prevention-related targets were specific, but limited to the provision of exercise-based programs that had limited capacity (e.g., 2500 individuals per year).19 While agencies and partners were mentioned in all documents, their involvement in the development of these documents and in the implementation of strategies to achieve the desired goals was often unclear. Our analysis underscores the importance of including a range of actors involved in falls prevention policies, fostering collaboration across sectors and establishing a clear plan that defines each actor’s role in enacting policy recommendations.
Figure 1. Upstream and downstream factors that impact on falls among community-dwelling older adults (click figure to enlarge)
Note: Figure 1 was developed by drawing from the findings of the content analysis of policy documents, the collaborative analysis guided by the PSCF framework, and our collective experiences and expertise across the fields of falls prevention research, public health, health policy, urban planning, aged care, health economics, housing, health inequities and advocacy for policy change.
Connections and boundaries: How are government departments, nongovernment organisations, industry, and community groups working together (e.g., siloed or well-connected)? What needs to change? How well do government stakeholders, nongovernment organisations, industry, and community groups trust each other and share information, data, and resources?
A range of stakeholders were mentioned across the documents, i.e., government departments, nongovernment organisations, industry and community groups. However, there is no clear evidence to suggest that these stakeholders are effectively collaborating and working together in a coordinated manner. While the engagement of communities with lived experience (e.g., older adults, carers) was mentioned at times, it was poorly defined and lacked specificity. The Council on the Ageing (a leading advocacy organisation for older Australians) was mentioned as a partner in only two of the eight documents.19,20 Our analysis supports the meaningful inclusion of such groups to provide further insights into promoting systems change and reducing the burden of falls in communities and society more broadly. Few documents explicitly discussed those likely to experience inequities, including Aboriginal and Torres Strait Islander people, those with disabilities, those living in rural and regional areas and those from multicultural backgrounds. Involving these populations and other actors (e.g., private health insurers) is imperative to identify interdependencies, define actor involvement and clearly define targets for intersectoral action while considering the unique contribution of each actor.
We were unable to conclude how well government stakeholders, nongovernment organisations, and industry and community groups share information, data, and resources on falls. To the best of our knowledge, there is no single repository to share information and data across local, state and federal governments, which indicates an area for improvement in information and data sharing across government levels. For instance, there is a lack of data monitoring in primary care, and it is often difficult to capture data on what happens after an older person has been hospitalised due to a fall. The National Health Survey does not currently include questions about falls. However, such data has relevance for future action plans.
Power and control dynamics: How much do the different policy actors within the policy community (government departments, non-government organisations, technical experts, and researchers) have real influence over intersectoral policy decisions, processes, plans, and options? How do different government departments share decision-making power around policies?
In assessing the influence of different policy actors within the falls prevention community and in light of the range of key stakeholders mentioned across the documents, our team concluded that no single group had enough influence to drive a national falls prevention policy on their own. For instance, despite two authors being established researchers in the field of falls prevention and undertaking leadership and advocacy roles (KD is President of the Australian and New Zealand Falls Prevention Society [ANZFPS] and CS is former ANZFPS President and lead of the NHMRC CRE in Prevention of Falls Injuries), fostering policy change in this space remains challenging. Other important policy changes in other fields21, together with our collaborative discussions, support the need for coordinated action across different government levels and both government and nongovernment sectors to tackle the problem, with a focus on establishing clear responsibilities for each. In Australia, the leadership of this coordinated action could sit under a particular institution or a task force group, ideally coordinated by the Australian Government Department of Health and Aged Care, which has an overarching national responsibility for falls prevention.
System regulations – Do any current policies or procedures get in the way of the overall goal of working towards achieving chronic disease prevention? If so, which ones need to change? What new policies are procedures are needed to support the overall goal? How does the current policy context motivate intersectoral action to create changes to facilitate systems changes?
While we could not identify specific policy barriers to falls prevention, our analysis identified factors to enable improved falls prevention policy. These include: i) tailored programs for both middle-aged and older-aged people; ii) interdisciplinary partnerships recognising falls as a multifactorial problem that overlaps with other health conditions (e.g., vision impairment, musculoskeletal problems, malnutrition); iii) inclusive mass media campaigns; iv) financial incentives to promote engagement in activities aligned with falls prevention; v) public and building design regulations/standards; vi) funding for non-pharmacological interventions such as community-based physical activity programs and allied health services; and vii) consideration of falls as a public health problem that calls for intersectoral action. None of the included policies focused solely on falls prevention, indicating that falls might not be perceived as a public health issue that requires a policy of its own.
Values and norms: What attitudes and values held by policy decision makers might obscure proposed changes?
When discussing attitudes and values held by policymakers that might obscure proposed changes, our team raised potential issues related to ageism and ableism. Most (83%) Australians agree that ageism exists in Australian society, and 64% of older people report being affected by ageism in the last 5 years.22 While these data focused mostly on interpersonal experiences with ageism, research suggests that Australian policy documents reflect institutional ageism. A critical discourse analysis of physical activity policy documents from 16 local government areas in Victoria, Australia, indicated that local government policies construct and perpetuate various stereotypes of older adults, portraying them as a financial burden.23 Likewise, a study in Queensland, Australia, indicated that spaces designed for older people reinforced historical legacies of separation from the community and stereotypes of older people as either ageless (appearing not to grow old) or dependent.24 Gendron et al., have advocated for initiatives and community-level interventions to challenge ageism and ableism, promoting inclusivity and reducing the stigma associated with ageing.25 This is supported by our analysis, which highlights the need to reflect on discourses that may underpin policy inaction in falls prevention – an ageist and ableist society is unlikely to prioritise such an issue. Our analysis suggests there is a need for policymakers to avoid assuming homogeneity among older people, as not all older adults are vulnerable and dependent. Thus, future policies targeting falls prevention may benefit from: i) attending to the unintended consequences of implicit and explicit ideas about ageing and ableism; and ii) considering a range of cohorts of older adults, as their contributions to, and demands on, life, health and policy budgets differ.
Another perception that might impede policy changes is the idea that falls are an ‘event’, rather than a chronic condition. In the documents we identified, falls appear to sit between injury and chronic disease, but in reality, are neither of them. Within this context, policymakers might not perceive falls and physical function as outcomes of interest, in contrast to more tangible and seemingly more severe outcomes such as high blood pressure or cancer recurrence. However, falls can be fatal2 and approximately one-third of falls can be prevented. Similarly, physical function has a significant impact on the health and wellbeing of older adults, with high physical function at 65-80 years being associated with a lower risk of falls, independence beyond 80 years, and improved mental health and cognition.26 Therefore, the results suggest that advocating for greater recognition of falls and physical function as important outcomes in falls prevention policies is warranted.
Systems interdependencies: What are the key leverage points for addressing the issue?
Drawing on our analysis of current policy documents targeting falls, our collaborative discussions, international models of good practice, recommendations from the WHO, and system change learnings from other fields, we propose eight key leverage points for addressing falls prevention as a critical public health issue:
- Establishing a multisectoral and interdisciplinary national falls prevention task force and coordination group that centres its efforts on community needs. This task force should collaborate to develop shared priorities, monitoring and reporting mechanisms to formalise accountability and responsibility through a national falls prevention strategy. Notably, co-production and collaboration between decision-makers and researchers are among the best predictors of research influencing policy and practice.27
- Integrating falls prevention goals and strategies into urban planning, transport and housing policies to create all-abilities accessible environments and individuals’ choices in transport and housing and to reduce environmental exposures that contribute to falls.
- Building a centralised repository for local and state-based falls prevention initiatives (e.g., community programs, care pathways). This repository would serve as a valuable resource and potentially include toolkits to support falls prevention efforts.
- Promoting discourses and actions addressing health inequities, stigma, ageism and ableism. These efforts would aim to challenge discriminatory attitudes and behaviours while fostering inclusivity and reducing the stigma associated with ageing and falls.
- Promoting physical activity opportunities to increase balance and functional strength across the lifespan.
- Adopting equitable policy design that ensures equal access to fall-prevention programs, such as through rental tenancy regulations or government grants that enable residents across housing tenures to implement measures and seek support.
- Allocating funding to expand on effective falls prevention programs and non-pharmacological interventions such as modifications to home and podiatric interventions for those with disabling foot pain.
- Capacity building in the health and aged care sectors to promote and incorporate falls prevention strategies in interactions with older people and their families. This will ensure that healthcare professionals are well-equipped to address falls prevention as an integral part of their practice.
Facilitating policy action
In this paper, we applied the first component of the PSCF framework to existing policies that encompass falls to reflect on and propose actions that may assist changes in falls prevention in Australia. Our analysis, guided by the questions in the systemic lens domain of the PSCF framework10, supports a coordinated and interdisciplinary approach that engages a range of stakeholders and sectors to develop and implement interventions that promote falls prevention in the Australian context. Such an approach is underpinned by system thinking, which is based on the premise that there are multiple, systemic, dynamic and interconnecting factors that impact health issues such as falls. Its value lies in acknowledging that is not possible to understand an issue by considering factors in isolation.7,28 Within this context, it is important to draw attention to policies that have structured the system (or not) in a way that leads to certain outcomes such as a high prevalence of falls. To the best of our knowledge, this is the first study to examine falls prevention in Australia from a systems perspective.
While we are attempting to make a meaningful contribution towards policy change in falls prevention, we acknowledge that this study is the first step. Engaging in research that seeks to prompt change requires ongoing cycles of reflection (both self-reflection and reflection of the research process), action, feedback and planning.29 To achieve impactful research, intersectoral collaboration and co-creating solutions with stakeholders is imperative to develop a shared understanding of the problem and its context, which in turn fosters change.7,28 Within this context, long-term and multipurpose spaces where researchers and policy actors share and test their understandings of policy issues are likely to be fruitful. Given that individual-level interventions have been shown to have short-term effects and strategies targeting structural, environmental and socioeconomic factors can be more cost-effective and impactful in other fields30, falls prevention interventions may be more impactful if policies target inequities and prompt action across sectors.
Limitations
This study has limitations that need to be considered. We searched policy documents that were publicly available when using ‘Google’, and only considered websites listed in the first 10 pages (i.e., approximately 100 websites per combination of keywords). While we attempted to minimise this risk by considering falls prevention policy documents that were known by falls experts in our team and searching falls in Australian government departments’ and agencies’ websites, it is possible some eligible documents were missed.
Implications
Our analysis and results support the creation of a centralised repository where all the information about local, state/territory and federal fall prevention programs and care pathways can be easily accessed by healthcare professionals and consumers while considering population diversity, individual needs and structural challenges (e.g., rental tenants). While face-to-face programs offer opportunities for social connection that extend beyond falls prevention, incorporating emerging technologies and innovative solutions can extend the reach of falls prevention efforts, particularly for those who live in areas where such programs are not available.
Future research could explore the views of different actors on governance related to falls, with a focus on what needs to change to achieve a national policy and who is responsible for such changes. Within this context, it would be important to involve those with different sources of power and influence in the system (for example, epistemic power [e.g., academics], moral power [e.g., nongovernmental organisations], and financial power [e.g., private health insurers]). In other Australian policy contexts, it has been suggested sharing power in decision-making and institutional mechanisms to enable intersectoral collaboration might be beneficial10 and this might also work in the context of falls prevention. Applying the other components of the PSCF to falls context and research (e.g., implementation focus, integrating systemic lens and implementation focus, developing a theory of systems change) is likely to provide further insights to inform policy action in falls prevention.
Conclusion
This analysis suggests a mismatch between the extent of the problems posed by falls, and the attention given to falls prevention in policy in Australia. With a rapidly ageing Australian population, it is clear that current approaches to health policy, particularly the lack of investment in prevention, are not sustainable. Mounting pressure on health services and increasing public interest in falls prevention may provide the impetus for a renewed focus on falls. We believe this project has highlighted the need for a systemic and collaborative approach to falls prevention, one that leverages the strengths and insights of various sectors and stakeholders. By taking this approach, we can address the current gaps in falls prevention policy and pave the way for more effective, sustainable, and equitable approaches to this pressing public health issue.
Acknowledgements
We thank Belinda Wang, Cameron Hicks and Dr Jane Elkington for assisting with the searches and data extraction.
KD is President and CS is an Executive Committee member of the ANZFPS.
This paper is part of a special issue of the journal focusing on: ‘Collaborative partnerships for prevention: health determinants, systems and impact’. The issue has been produced in partnership with the Collaboration for Enhanced Research Impact (CERI), a joint initiative between The Australian Prevention Partnership Centre and NHMRC CREs. The Prevention Centre is managed by the Sax Institute in collaboration with its funding partners.
Peer review and provenance
Externally peer reviewed, invited.
Copyright:
© 2024 Costa et al. This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International Licence, which allows others to redistribute, adapt and share this work non-commercially provided they attribute the work and any adapted version of it is distributed under the same Creative Commons licence terms.
References
- 1. Li F, Fisher KJ, Harmer P, McAuley E, Wilson NL. Fear of falling in elderly persons: association with falls, functional ability, and quality of life. J Gerontol B Psychol Sci Soc Sci. 2003;58(5):P283–90. CrossRef | PubMed
- 2. Australian Institute of Health and Welfare. Falls in older Australians 2019–20: hospitalisations and deaths among people aged 65 and over. Canberra: AIHW; 2022 [cited 2024 Feb 06]. Available from: www.aihw.gov.au/reports/injury/falls-in-older-australians-2019-20-hospitalisation/contents/summary
- 3. World Health Organization. Step safely: strategies for preventing and managing falls across the life course. Geneva: WHO; 2021 [cited 2024 Feb 06]. Available from: iris.who.int/bitstream/handle/10665/340962/9789240021914-eng.pdf?sequence=1
- 4. Mabry PL, Marcus SE, Clark PI, Leischow SJ, Méndez D. Systems science: a revolution in public health policy research. Am J Public Health. 2010;100(7):1161–3. CrossRef | PubMed
- 5. Carey G, Malbon E, Carey N, Joyce A, Crammond B, Carey A. Systems science and systems thinking for public health: a systematic review of the field. BMJ Open. 2015;5(12):e009002. CrossRef | PubMed
- 6. Allender S, Brown AD, Bolton KA, Fraser P, Lowe J, Hovmand P. Translating systems thinking into practice for community action on childhood obesity. Obes Rev. 2019;20 Suppl 2(Suppl 2):179–84. CrossRef | PubMed
- 7. Davis AC, Stroink ML. The relationship between systems thinking and the new ecological paradigm: systems thinking and environmental worldview. Systems Research and Behavioral Science. 2016;33(4):575–86. CrossRef
- 8. Astbury CC, Lee KM, McGill E, Clarke J, Egan M, Halloran A, et al. Systems thinking and complexity science methods and the policy process in non-communicable disease prevention: a systematic scoping review. Int J Health Policy Manag. 2023;12:6772. CrossRef | PubMed
- 9. Haynes A, Rychetnik L, Finegood D, Irving M, Freebairn L, Hawe P. Applying systems thinking to knowledge mobilisation in public health. Health Res Policy Syst. 2020;18(1):134. CrossRef | PubMed
- 10. Pescud M, Rychetnik L, Allender S, Irving MJ, Finegood DT, Riley T, et al. From understanding to impactful action: systems thinking for systems change in chronic disease prevention research. Systems. 2021;9(3):61. CrossRef
- 11. Delbaere K, Elkington J, Lord SR, Batchelor F, Sturnieks DL, Sherrington C. The rising cost of falls – health researchers are calling for action. Australas J Ageing. 2022;41(4):487–9. CrossRef | PubMed
- 12. Buse K, Mays N, Walt G. Making health policy. 2nd ed. Maidenhead, England: McGraw-Hill; 2012.
- 13. Department of Health and Aged Care. National preventive health strategy, 2021–2030. Canberra: Australian Government; 2021 [cited 2024 Feb 6]. Available from: www.health.gov.au/resources/publications/national-preventive-health-strategy-2021-2030?language=en
- 14. Department of Health and Aged Care. National Injury Prevention Strategy 2020–2030. Draft for consultation. Canberra: Australian Government; 2020 [cited 2024 Feb 6]. Available from: consultations.health.gov.au/population-health-and-sport-division/national-injury-prevention-strategy_/user_uploads/national-injury-prevention-strategy-draft-for-consultation-may-2020-1.pdf
- 15. Australian Commission on Safety and Quality in Health Care. The national safety and quality health service (NSQHS) standards. Second edition. Sydney: ACSQHC; 2021 [cited 2024 Feb 06]. Available from: www.safetyandquality.gov.au/standards/nsqhs-standards
- 16. Government of Western Australia Department of Health. Western Australian health promotion strategic framework 2022–2026. Perth, WA: Government of Western Australia; 2022 [cited 2024 Feb 06]. Available from: www.health.wa.gov.au/~/media/Corp/Documents/Reports-and-publications/HPSF/Health-Promotion-Strategic-Framework-2022-2026.pdf
- 17. WA Country Health Service. WA Country Health Service strategy for older people 2022–2027. Perth, WA: Government of Western Australia; 2022 [cited 2024 Feb 06]. Available from: www.wacountry.health.wa.gov.au/~/media/WACHS/Documents/About-us/Publications/Strategic-plans/Health-Strategy-for-Older-People-2022-27.PDF.
- 18. South Western Sydney Local Health District. Strategic & healthcare services plan. Strategic priorities in health care delivery to 2021. Sydney, NSW: SWSLHD; 2013 [cited 2024 Feb 06]. Available from: www.swslhd.health.nsw.gov.au/pdfs/SWSLHD_Strategic_Priorities_to_2021.pdf
- 19. Department of Communities and Justice. Ageing well in NSW. Action plan 2023–2024. Sydney, NSW: NSW Government; 2023 [cited 2024 Feb 06]. Available from: dcj.nsw.gov.au/documents/community-inclusion/seniors/Ageing_Well_Action_Plan_2023-24_FA_300123.pdf
- 20. Primary Health Networks Central Queensland. Ageing well in our region: a healthy ageing strategy 2022–2027. PHN Central Queensland, Wide Bay, Sunshine Coast, Queensland; 2022 [cited 2024 Feb 06]. Available from: c2coast.org.au/wp-content/uploads/2022_PHN_004_CQWBSCPHN-Healthy-Ageing-Strategy-2022-2027_v1.0.pdf
- 21. Amri M, Chatur A, O'Campo P. An umbrella review of intersectoral and multisectoral approaches to health policy. Social Science & Medicine. 2022;315:115469. CrossRef | PubMed
- 22. Australian Commission Human Rights. What's age got to do with it? A snapshot of ageism across the Australian lifespan. Sydney, NSW: ACHR; 2021 [cited 2024 Feb 06]. Available from: humanrights.gov.au/our-work/age-discrimination/publications/whats-age-got-do-it-2021
- 23. Butson M, Jeanes R, O’Connor J. Identifying ageism within Australian local government physical activity policy: a critical discourse analysis. J Aging Phys Act. 2023:32(1):34–42. CrossRef | PubMed
- 24. Petersen M, Warburton J. Residential complexes in Queensland, Australia: a space of segregation and ageism? Ageing & Society. 2012;32(1):60–84. CrossRef
- 25. Gendron T, Camp A, Amateau G, Mulle M, Jacobs K, Inker J, et al. The next critical turn for ageism research: The intersections of ageism and ableism. Gerontologist. 2024;64(2):gnad062. CrossRef | PubMed
- 26. Falls in older people: risk factors, strategies for prevention and implications for practice. 3rd ed. Cambridge, UK: Cambridge University Press; 2021.
- 27. Gagliardi AR, Berta W, Kothari A, Boyko J, Urquhart R. Integrated knowledge translation (IKT) in health care: a scoping review. Implement Sci. 2016;11:38. CrossRef | PubMed
- 28. Bagnall AM, Radley D, Jones R, Gately P, Nobles J, Van Dijk M, et al. Whole systems approaches to obesity and other complex public health challenges: a systematic review. BMC Public Health. 2019;19(1):8. CrossRef | PubMed
- 29. Riley T, Hopkins L, Gomez M, Davidson S, Chamberlain D, Jacob J, et al. A systems thinking methodology for studying prevention efforts in communities. Systemic Practice and Action Research. 2021;34(5):555–73. CrossRef
- 30. Jørgensen T, Capewell S, Prescott E, Allender A S, Sans S, Zdrojewski T, et al. Population-level changes to promote cardiovascular health. Eur J Prev Cardiol. 2013;20(3):409–21. CrossRef | PubMed