Abstract
This year, 2021, marks the 40th anniversary of the iconic Slip! Slop! Slap! campaign which launched Australia’s status as a global leader in skin cancer prevention. Since the campaign first aired in the summer of 1980–81, notable successes have been achieved, with melanoma rates declining in younger age groups. While skin cancer prevention is rightly considered a triumph of Australian public health, challenges remain. Australia still has one of the highest rates of skin cancer in the world, with about 2000 deaths per year from the disease. Skin cancer also presents the highest cost burden to the health system of any cancer type. Despite this, government investment at the national level is lacking. It is more difficult than ever to collect valuable representative national data on population skin cancer prevention behaviours to underpin and evaluate programs, as the methodology used previously has become unfeasible. There has not been a national skin cancer prevention mass-media campaign for over a decade, indicating complacency from policy makers. State and territory governments could also do more to implement evidence-based policies aimed at protecting children from ultraviolet radiation. This paper sets out Australia’s skin cancer prevention landscape in 2021, and makes the case for a renewed focus from government on sun protection to safeguard the significant gains made over four decades and to protect future generations from an almost entirely preventable cancer.
Full text
Introduction
Ultraviolet radiation (UVR) from the sun is the primary cause of skin cancer: it is estimated that up to 95% of melanomas and 99% of non-melanoma skin cancers (NMSC) in Australia are caused by overexposure to UVR.1,2 Australians with the fairest skin types are particularly susceptible to the danger presented by the country’s high-UVR environment.3 Children and young adults are also at high risk, with UVR exposure during a person’s first 18 years of life the most critical for cancer-causing skin damage.4
The fact that skin cancer is largely caused by UVR means it is also preventable by using good sun protection consisting of a combination of five measures: clothing, sunscreen, broadbrim hats, shade and sunglasses. This is encapsulated by the phrase ‘Slip, Slop, Slap, Seek, Slide’. The preventability of skin cancer presents a considerable opportunity to implement effective policies and campaigns. The iconic Slip! Slop! Slap! campaign in 1980–81, followed by a comprehensive, evidence-based SunSmart program in 1988, heralded a new era for skin cancer prevention in Australia (Figure 1). SunSmart initiatives include mass-media public education campaigns, a schools and early childhood membership program, workplace education and health professional training. This program has contributed to population-wide improvements in sun protection behaviours since the 1980s.5 The global influence of our efforts cannot be underestimated. Many countries with predominantly fair-skinned populations have seen Australia as a world leader in skin cancer prevention. Some countries have adopted the use of our “SunSmart” and “Slip, Slop, Slap” slogans, while many other countries, including New Zealand, US, UK, Ireland and Denmark, have applied the learnings based on Australia’s experience.
Figure 1. Sid Seagull, mascot from the original Slip! Slop! Slap! Campaign in 1981 (click to enlarge)
The SunSmart program has also been instrumental in achieving a considerable cultural shift towards sun protection norms in pre- and primary school–age children, as well as schools and workplaces adopting a sun protection policy.6 Government policy changes including Goods and Services Tax (GST) being removed from sunscreen in 2001, tax deductions on sun-protective items for outdoor workers being introduced in 2002, and the nationwide ban on commercial solariums implemented in 2015 have also provided a supportive environment for limiting over-exposure to UVR, and will likely contribute to future reductions in skin cancer incidence. Compared with Australia and Brazil (which has also banned solariums), other countries have less stringent regulations in place relating to indoor tanning, such as restricting use for those under 18 years.
Melanoma incidence in Australia is projected to decline over the coming years, though it continues to increase in other countries.7 Environmental and behavioural changes achieved since the 1980s have likely contributed to the decline in younger Australians8 – the cohort who have had the benefit of skin cancer prevention programs for most of their lives.
Skin cancer prevention has also been found to offer strong economic benefits. At the national level, prevention programs have been estimated to deliver a return on investment of $3.20 per dollar spent.9 Recent modelling has shown that if investment is made in preventing skin cancer, compared to no investment, cost savings over the next 10 years can amount to $3.63 billion based on Australia’s current population of 25.6 million.10 We expect these cost savings will increase over time, highlighting the significant benefit of investing in mass-media public education campaigns. Cancer Council has estimated the cost of a properly funded and evaluated campaign at $20 million a year11 – just over 1% of the annual cost of skin cancer treatment.
Complacency means there’s more to do
Despite our achievements, skin cancer prevention in Australia seems to have become a victim of its own success. Given the impact of the SunSmart program over the decades, from school children wearing hats to ‘Slip! Slop! Slap!’ becoming part of the national vocabulary, it is tempting to assume the problem is solved. However, there has been no national investment in skin cancer prevention initiatives – including public education campaigns – in Australia for more than a decade. Encouragingly, following advocacy from leading skin cancer organisations, a commitment to deliver a national skin cancer prevention mass-media campaign was recently made in the draft National Preventive Health Strategy.12
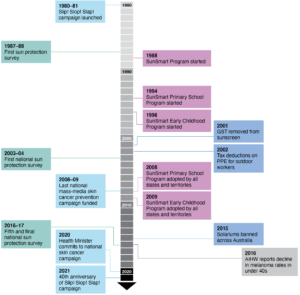
The lack of national investment is particularly alarming because sun-protective behaviours increase as skin cancer prevention campaign advertising increases, and they decrease when advertising is absent.13 Furthermore, solar UVR presents a constant cancer risk to Australians, requiring daily action for most of the year at the individual level to prevent overexposure. Not only is it important to prompt the timely use of sun protection for those already familiar with the need to do so, but it is also essential to introduce new generations and migrants to Australia to sun protection as a social norm. Efforts to maintain and improve sun protection behaviours therefore require sustained funding to be effective (Figure 2).
Figure 2. A 40-year history of skin cancer prevention in Australia (click to enlarge)
GST = goods and services tax; PPE = personal protective equipment; AIHW = Australian Institute of Health and Welfare
Why do we need a renewed focus on skin cancer prevention?
Ongoing threat to health
Australia still has one of the highest rates of skin cancer in the world14, with 14 846 melanomas diagnosed in 2017.15 It is estimated that cases of NMSC exceed all other cancer types combined8, with Medicare data showing there were more than 1 million treatments for NMSC in 2020.16 There are about 2000 deaths from all skin cancer types annually.17 This health burden necessitates a renewed focus on skin cancer prevention policy from governments, without which the gains made to date are at risk, with the threat of melanoma rates increasing in the future.
Spiralling economic costs
In addition to the considerable health impacts of skin cancer, the economic cost is enormous. The Australian Institute for Health and Welfare found skin cancer (melanoma and NMSC combined) to cost $1.68 billion in 2018–19.18 It is the most expensive cancer type to treat, and overexposure to solar UVR is also estimated to account for the highest amount of spend on cancer that can be attributed to a risk factor, at 31% – higher even than tobacco use (24%).19 These high costs make it even more incredible that there is currently no government investment in skin cancer prevention at the national level, especially as it is likely that expenditure on treatments will rise even further as new, more expensive therapies for melanoma are subsidised on the Australian Government Pharmaceutical Benefits Scheme. The economic benefits of investing in prevention are only likely to increase in this context, meaning skin cancer prevention offers governments excellent value for money in the long term.
Threats to population monitoring
We know prevention efforts have resulted in improved sun-protection behaviours and likely contributed to a reduction in melanoma incidence due to evidence from regular, large-scale population monitoring surveys conducted since the summer of 1987–88 – before the start of the SunSmart program. The National Sun Protection Survey (NSPS) was the primary method of collecting data to inform and evaluate skin cancer prevention initiatives, and report on behavioural trends in Australia. Conducted triennially between the summers of 2003–2004 and 2016–2017, the NSPS was based on Victorian surveys collected from 1987–88 onwards. Some iterations of the national survey were jointly funded by government agencies and Cancer Council Australia, with others – including the most recent survey – funded solely by Cancer Council. Declining response rates to telephone surveys have had a devastating impact on the ability to conduct representative population monitoring with response rates falling to only 10% in the summer of 2016–17, rendering the telephone-based methodology unfeasible.20
The NSPS provided valuable insights into Australians’ sun protection knowledge, attitudes and behaviours, with the longevity and consistency of the survey allowing for reporting of trends over time. Importantly, the NSPS methodology was designed to collect behavioural data over six summer weekends for each survey, limiting the influence of variable weather conditions on sun protection behaviours when comparing across survey years. The data were used by national cancer organisations to track Australia’s record on skin cancer prevention and inform policy and program direction. The loss of the survey has therefore left a huge gap in our understanding and monitoring of skin cancer prevention in Australia.
There are three complementary ways in which this gap in knowledge may be addressed: firstly, through government health surveys at the state and federal level which have higher response rates, although any skin cancer prevention measures that are included will be subject to survey length constraints so only critical questions would be prioritised. Secondly, studies in which sun-protection behaviours are observed in real-world settings could be used, although it is not possible to observe sun-protection behaviours in private settings. Although this method is not suitable for generating population estimates of sun-protection behaviours, it could nonetheless provide more detail on sun protection in outdoor community environments. Thirdly, online surveys can be used, with priority given to online panels that offer a probability-based sampling frame. However, there are currently limited options for these types of panels and their methodology does not allow data to be collected over an extended time period, which is crucial to reducing weather variability for monitoring sun protection behaviour trends over time. Unfortunately, even if all three methods are used, it is unlikely they would fully compensate for the gap left by the NSPS. In addition, all these methods require sufficient ongoing funding so a concerted commitment from government and not-for-profit organisations is needed.
Adolescents present an ongoing challenge
Adolescents have long been the SunSmart program’s toughest audience to reach.6 Although preference for a tan among teenagers has reduced since 2003, improvement has stalled in recent years with 38% still preferring a tan in the summer of 2016–17.21 Concerningly, sunburn incidence did not decrease among adolescents since 2003–04 with 26% of teens reporting being sunburnt on summer weekends in 2016–17.20
Although we have seen cultural shifts towards sun protection in primary schools, early childhood centres and workplaces over the last few decades, the same cannot be said for secondary schools. Secondary school teachers cite factors such as competing priorities, attempts to encourage independence among students, and peer pressure as barriers to implementing sun protection.22 Clearly, more action is needed by schools, supported by state education departments, to implement policies and practices that protect adolescents from UVR.
Opportunities to put skin cancer prevention back on the political agenda
Skin cancer prevention interventions present an opportunity for presiding governments for three key reasons. Firstly, children’s susceptibility to the skin damage caused by UVR makes them an excellent target for skin cancer prevention interventions. Policies which protect the health of the younger generation usually attract considerable public support. Secondly, Australia is free of active industry opposition to skin cancer prevention initiatives since the ban on commercial solariums. This is in direct contrast to other areas of cancer prevention like tobacco, alcohol and obesity, where strong industry opposition to public health measures must be navigated with considerable effort. Thirdly, the health and economic benefits of investing in skin cancer prevention are well established, making properly designed policies both effective and cost-effective.
A comprehensive strategy comprising public education, robust data collection and regulatory measures aimed at protecting children presents the best opportunity to maximise gains in skin cancer prevention.
A national skin cancer prevention campaign for Australia
Encouragingly, after more than a decade of inaction, there has been a recent resurgence in interest in skin cancer prevention policies at the national level. Ahead of the last national election, the former Leader of the Opposition announced a 2-year, $8.6 million skin cancer prevention campaign23 – the first commitment to a national sun protection campaign from a major political party since the last mass-media campaign ran in 2008–09. However, as his party was not elected to government, the commitment was not enacted.
The current national Health Minister has recently committed to the delivery of a national skin cancer prevention campaign in the government’s draft National Preventive Health Strategy.12 Given the positive impact of mass-media campaigns on sun protective behaviours, the priority must now be to ensure this commitment is acted upon with sufficient funding to achieve and sustain behaviour change and deliver robust evaluation.
The need for robust population monitoring
The demise of the NSPS means a combination of complementary methods is required to fill the gap in data on sun-protection knowledge, attitudes and behaviour which is essential to underpin skin cancer prevention initiatives. Cancer Council plans to continue the collection of observational data on sun-protection behaviours24, and data on attitudes and knowledge through representative online surveys, however the only way to now collect high-quality behavioural data on sun protection is via government population surveys that can achieve high response rates. Given skin cancer’s significance as Australia’s national cancer, and the considerable health and economic burdens it presents, data on sun-protection behavioural measures should be prioritised for collection in government surveys over the long term to provide vital population-level data for monitoring of behavioural risk factors for skin cancer.
Protecting children
Additional evidence-based regulatory measures should be implemented by governments to protect children from overexposure to UVR as part of a comprehensive strategy.
Firstly, state governments should mandate an evidence-based sun protection policy in secondary schools. Decades of experience from the SunSmart program shows that voluntary policies have not worked in the secondary school setting. If we are serious about our duty of care towards Australian teens, we should mandate their protection from UVR in the same way we ban the sale of other carcinogens like tobacco and alcohol, and require the use of seatbelts and bicycle helmets. In workplaces, UVR is considered an occupational health and safety risk, and employers and employees share a duty to take reasonable steps to protect staff. This means we are in the unacceptable situation where a parent could be better protected from a known carcinogen at work than their child is in the playground at school. Sun protection should be taken as seriously in secondary schools as it is in workplaces.
Secondly, the provision of shade in public settings is a relatively easy policy win. When shade is available, adolescents use it25, and it does not require the level of effort needed to implement other sun protection measures (clothing, hats, sunscreen and sunglasses). Natural shade also provides environmental benefits. The Victorian and Queensland Governments currently deliver shade grant programs – albeit with varying levels of funding. Pleasingly, shade provision in schools in Victoria has been prioritised in a push towards outdoor learning in response to the coronavirus disease 2019 (COVID-19) pandemic. Other state governments should follow their lead in delivering long-term funding for what is arguably the simplest sun protection measure in their communities.
Skin cancer prevention in Australia: 40 years of progress – but the work is not done
The consistency of skin cancer prevention messages since the early 1980s has led to improvements in sun-protection behaviours in Australia and paved the way for other countries to learn from Australia’s success. Given the time lag between overexposure to UVR and a diagnosis of skin cancer, we are now starting to see the positive impacts of four decades of work in reduced incidence in younger age groups. However, Australia’s governments need to eschew complacency and renew their focus on implementing effective skin cancer prevention policies. A comprehensive strategy of mass-media campaigns, robust data collection and regulatory measures to safeguard children presents the best opportunity to consolidate the gains made to date and drive further progress in protecting future generations from an almost entirely preventable cancer. When it comes to skin cancer prevention, Australia knows what to do. Now’s the time to do it.
Acknowledgements
We would like to acknowledge our colleagues: Justine Osborne, SunSmart Schools and Early Childhood Coordinator, for her advice on the history of the SunSmart program; and Stephanie Cowdery, SunSmart Research and Evaluation Officer, for her assistance in preparing the manuscript. We also acknowledge Australia’s skin cancer prevention community whose work over 40 years has contributed to reductions in incidence and mortality from the disease.
This paper will be published as part a special issue on skin cancer prevention in 2022. The issue is being supported by and developed in partnership with Cancer Council Australia.
Peer review and provenance
Externally peer reviewed, invited.
Copyright:
© 2021 Walker et al. This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International Licence, which allows others to redistribute, adapt and share this work non-commercially provided they attribute the work and any adapted version of it is distributed under the same Creative Commons licence terms.