Abstract
Early childhood provides an opportunity to support parents to promote a range of healthy behaviours at a time of high engagement with family-focused health services. The Infant Program is believed to be the first of its kind to address healthy behaviours and obesity risk in the first year of life using a universally delivered service. The program is an efficacious, low-cost intervention, and many lessons have been learnt across the journey from a randomised controlled trial to small-scale community implementation. The evolution of the Infant Program highlights the value of applying a translational research process to best position interventions to be implemented at scale. It also illustrates the benefits that a sequential approach, a receptive environment and system-level support provide when seeking to integrate new interventions into routine health service delivery. Understanding these processes and factors leads to a better appreciation of the role each step plays in implementing population health interventions at scale.
Full text
Introduction
Early adiposity has lifelong health and economic consequences, with prevention a national and international priority.1 In Australia, a minority of children meet dietary, physical activity or sedentary behaviour guidelines2, and one in five (21.2%) are overweight or obese by the age of 5 years.2 Most population-based interventions to improve health behaviours in early life occur via settings outside the home, such as childcare. However, with only 16% of Australian children younger than 1 year of age attending childcare3, the main influence at this time remains the family and home environment.
Family-focused health services are well placed to support parents to develop knowledge, skills and confidence regarding child health behaviours, and parents are highly receptive to such support.4 In Victoria, the universal free Maternal and Child Health (MCH) service provides 10 consultations between birth and age 3.5 years, with 80–90% attendance during the first 12 months.5 This means early childhood provides an opportunity to support parents when engagement with MCH services is high. However, the provision of such support through the process of translating efficacious research trials into ‘real-world’ practice settings is limited. Little evidence is available as to what is needed for the successful dissemination, implementation and scale-up of interventions to address this research–practice gap.
The Infant Program: from trial to translation
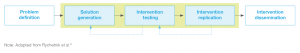
The Infant Program is believed to be the first of its kind to address obesity risk in the first year of life using a universally delivered service. Many lessons have been learnt about the translation from randomised controlled trial (RCT) to small-scale community implementation. This process is illustrated below using a translational research framework comprising five stages: problem definition; solution generation; intervention testing; intervention replication; and intervention dissemination (Figure 1).6
Figure 1. Translation processes to support evidence based practice and policy (click to expand)
Problem identification and solution generation
The concept and development of the Infant Program was informed by systematic reviews and primary studies.7 Evidence highlighted that obesity-promoting behaviours are established early in life; parents play a primary role in shaping these behaviours during infancy; intervening before these behaviours (and parents’ responses to them) are established is likely to be effective (anticipatory guidance); and the social environment provided by parent groups may facilitate and support uptake of health promotion messages.7 Evidence also supported the proposition that the delivery of health behaviour education was feasible through existing MCH infrastructures.7
Intervention testing
The Infant Program was originally tested through a cluster RCT.7 Using existing new parent groups established by Victoria’s universal MCH services when infants are aged around 3 months, first-time parents were offered six 2-hour sessions over 15 months. The sessions, delivered by dietitians using an anticipatory guidance approach, focus on parental knowledge, skills and social support around infant feeding, diet, physical activity and sedentary behaviours. The program achieved high acceptance and uptake.8
Child outcomes after the intervention showed children watched 25% less television, consumed 25% fewer sweet snacks and had improved dietary quality, and children of younger or less educated mothers drank more water and ate more vegetables than before the intervention.8 Maternal outcomes included decreased consumption of high-energy snacks, processed and high-fat foods; and significant improvements in knowledge of child feeding messages, intentional modelling of healthy eating, self-efficacy and important feeding practices to promote healthy eating.9 Beneficial intervention effects were not observed in fathers, indicative of the program engaging mothers as the point of contact. All results were considered clinically meaningful.
The Infant Program did not achieve the primary outcome of reducing body mass index (BMI). Importantly, however, when data from the Infant Program was pooled with three other Australasian early obesity prevention trials, the hypothesis that early childhood interventions could effect a significant and clinically meaningful change in child BMI was confirmed.10 Follow-up of participants at 2 years and 3.5 years post intervention confirmed beneficial maternal and child outcomes.8
The RCT demonstrated that the Infant Program was an efficacious, low-cost intervention that was well received across various demographic and socio-economic groups, suggesting that it could feasibly be translated to real-world settings.
Intervention replication and dissemination
The Infant Program RCT was delivered by dietitians. Given the high frequency of parent contact with MCH nurses in Victoria, an additional study explored the scope of MCH nurses to influence obesity prevention practices.11 Almost one-quarter of MCH nurses reported never/rarely using growth charts to identify those at risk of overweight, reflecting a lack of confidence in addressing the issue of weight with parents. The majority of MCH nurses reported routinely providing advice on infant feeding; less than half routinely promoted active play; and only one-third discussed limiting sedentary behaviour. MCH nurses were considered well placed to promote healthy weight gain within their role, but required additional support to incorporate this into routine consultations.11
Enhancements have been made to the content and delivery of the Infant Program. The Infant Extend Study explored providing program content through dedicated website pages, and introduced a closed and mediated Facebook group.12 Those who joined the Facebook group had more favourable outcomes in terms of BMI z-score (a measure of relative weight adjusted for child age and sex); intakes of vegetables, water and noncore sweet and savoury snacks; television viewing; and physical activity, with significantly higher fruit intake.12 The Facebook group was considered an effective and efficient means of communicating with participants, especially for administrative tasks (such as organising group sessions) and reinforcing program messages, as well as providing social support and a trusted source of information sharing.12 In parallel research, a smartphone app to promote healthy infant feeding behaviours has been shown to be a feasible and acceptable mode for delivering an obesity prevention intervention to parents.13
Given the program’s reliance on voluntary attendance, insights regarding program engagement and retention have also been investigated through qualitative interviews with program service providers and participants with varying patterns of attendance. Enablers and barriers to attendance were linked to personal, organisational and program factors. Findings will inform strategies to address modifiable barriers, for example, early program promotion during pregnancy, flexible modes of delivery using web and app-based technologies, and codesign and referral through interagency collaborations to reach vulnerable parents.4
In 2013, the Infant Program was selected by the Victorian Department of Health and Human Services as part of the Healthy Together Victoria (HTV) Initiative for small-scale implementation across select communities. Factors influencing translation of the program into routine practice were explored in sites implementing the program for at least 6 months.14 The program was well accepted and adopted by MCH nurses and health professionals. Potential barriers to program integration included a high administrative burden of delivering the program; challenges for facilitators accessing face-to-face training; and limited administrative time and confidence to evaluate program delivery. A major concern was funding stability, given that ongoing national-, state- or local-level program funding was unlikely. Embedding program delivery into existing service infrastructure was deemed critical, but challenging.14 In 2015, national preventive health funding ceased, impacting the HTV initiative, and providing an opportunity to examine factors contributing to sustained program implementation. A multisite qualitative exploratory study is currently under way to investigate barriers and enablers to sustained implementation across local government areas in Victoria.
An essential component of intervention replication and dissemination is the intervention’s capacity to be scaled up to achieve a population-level effect while retaining its effectiveness. ‘At scale’ implementation of the Infant Program is currently being planned, including evaluating the effectiveness and cost-effectiveness of implementation. In line with recommendations for scaling-up of population health interventions, multiple community, local government and state-level stakeholders will be engaged, with a focus on the reorientation of health service capacity to embed program delivery into routine practice.
Conclusion
The evolution of the Infant Program highlights the value provided by the translational research process. Being adaptive to research learnings and accommodating these into intervention design and delivery has placed the program in a strong position to be implemented at scale. Barker et al.15 describe three important factors to support successful intervention scale-up: a sequential approach, a receptive environment and system-level support (infrastructure, and human capacity and capability such as leadership). The development of the Infant Program illustrates how these factors have been considered and incorporated for real-world implementation. Understanding these processes and factors leads to a better appreciation of the role each step plays in implementing population health interventions at scale.
Acknowledgements
The Infant Program RCT and follow-up studies were funded by National Health and Medical Research Council (NHMRC) Project Grants; and the Infant Extend Study funded by a World Cancer Research Fund Grant. PL is funded through the NHMRC Centre of Research Excellence for Early Prevention of Obesity in Childhood. RL held an NHMRC Early Career Researcher Fellowship when conducting the Infant Program implementation study. KH holds an Australian Research Council Future Fellowship and an Honorary National Heart Foundation of Australia Future Leader Fellowship.
Peer review and provenance
Externally peer reviewed, commissioned.
Copyright:
© 2019 Love et al. This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International Licence, which allows others to redistribute, adapt and share this work non-commercially provided they attribute the work and any adapted version of it is distributed under the same Creative Commons licence terms.
References
- 1. WHO. Report of the Commission on Ending Childhood Obesity. Geneva: World Health Organisation; 2016 [cited 2018 Jul 16]. Available from: www.who.int/end-childhood-obesity/final-report/en/
- 2. ABS. National Health Survey First Results, 2014–15. Canberra: Australian Bureau of Statistics; 2015 [cited 2018 Jul 16]. Available from: www.abs.gov.au/ausstats/[email protected]/Lookup/by%20Subject/4364.0.55.001~2014-15~Main%20Features~About%20the%20National%20Health%20Survey~3
- 3. Baxter J, Hand K. Access to early childhood education in Australia research report 24. Melbourne: Australian Institute of Family Studies; 2013 [cited 2018 Jul 16]. Available from: aifs.gov.au/sites/default/files/publication-documents/rr24.pdf
- 4. Love P, Laws R, Litterbach E, Campbell KJ. Factors influencing parental engagement in an early childhood obesity prevention program implemented at scale: the Infant Program. Nutrients. 2018;10(509):1–19. CrossRef | PubMed
- 5. Victoria State Government Education and Training. Maternal and child health services annual report: 2015–2016 statewide. Melbourne: Victoria State Government; 2018 [cited 2018 Jul 16]. Available from: www.education.vic.gov.au/Documents/childhood/providers/support/2015-16VictoriaStatewidereport.pdf
- 6. Rychetnik L, Bauman A, Laws R, King L, Rissel C, Nutbeam D, et al. Translating research for evidence-based public health: key concepts and future directions. J Epidemiol Community Health. 2012;66(12):1187–92. CrossRef | PubMed
- 7. Campbell KJ, Hesketh KD, Crawford D, Salmon J, Ball K, McCallum Z. The Infant Feeding Activity and Nutrition Trial (INFANT): an early intervention to prevent childhood obesity cluster-randomised controlled trial. BMC Public Health. 2008;8(103):1–9. CrossRef | PubMed
- 8. Hesketh KD, Campbell KJ, Salmon J, McNaughton SA, McCallum Z, Cameron A, et al. The Melbourne Infant Feeding, Activity and Nutrition Trial (InFANT) program follow-up. Contemp Clin Trials. 2013;34:145–51. CrossRef | PubMed
- 9. Spence AC, Campbell KJ, Crawford D, McNaughton SA, Hesketh KD. Mediators of improved child diet quality following a health promotion intervention: the Melbourne InFANT program. Int J Behav Nutr Phys Act. 2014;11(137):1–11. CrossRef | PubMed
- 10. Askie L, Martin A, Espinoza D, Campbell KJ, Daniels LA, Hesketh KD et al. What does the EPOCH (early prevention of obesity in childhood) prospective meta-analysis tell us about early life obesity prevention? Obes Res Clin Pract. 2014;8:3–4. CrossRef
- 11. Laws RA, Campbell KJ, van der Pligt P, Ball K, Lynch J, Russell G, et al. Obesity prevention in early life: an opportunity to better support the role of maternal and child health nurses in Australia. BMC Nurs. 2015;14(26):1–14. CrossRef | PubMed
- 12. Downing KL, Campbell KJ, van der Pligt P, Hesketh KD. Facilitator and participant use of Facebook in a community-based intervention for parents: the InFANT Extend program. Child Obes. 2017;13(6):443–54. CrossRef | PubMed
- 13. Laws RA, Denney-Wilson EA, Taki S, Russell C, Zheng M, Litterbach E, et al. Key lessons and impact of the Growing Healthy mHealth Program on milk feeding, timing of introduction of solids and infant growth: quasi-experimental study. JMIR Mhealth Uhealth. 2018;6(4):e78:1–17. CrossRef | PubMed
- 14. Laws RA, Hesketh KD, Ball K, Cooper C, Vrljic K, Campbell KJ. Translating an early childhood obesity prevention program for local community implementation: a case study of the Melbourne InFANT program. BMC Public Health. 2016;16(748):1–15. CrossRef | PubMed
- 15. Barker PM, Reid A, Schall MW. A framework for scaling up health interventions: lessons from large-scale improvement initiatives in Africa. Implement Sci. 2016;11(12):1–11. CrossRef | PubMed